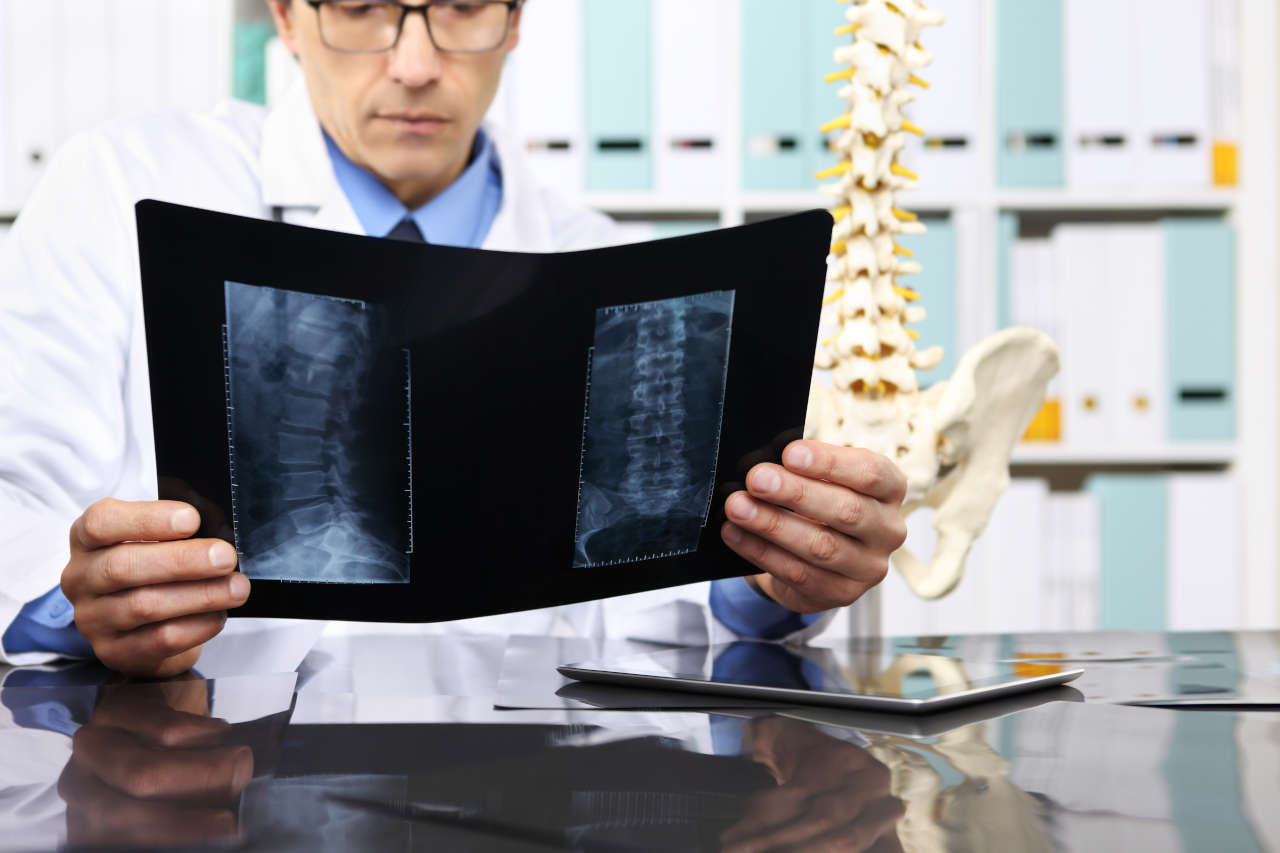
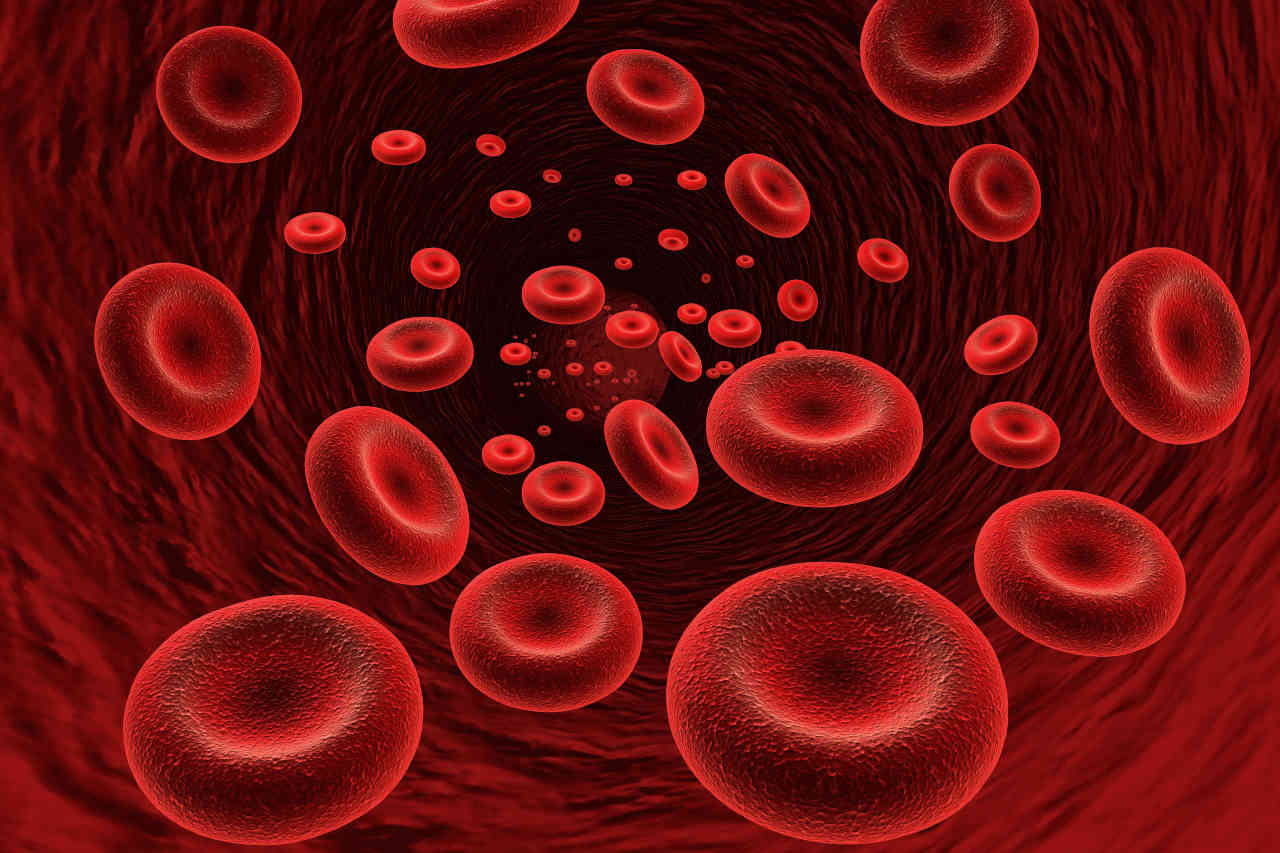
Autoimmune hemolytic anemia is a rare medical condition where the body’s own immune system attacks its red blood cells by mistake and destroys them. Red blood cells carry oxygen in your body. As a result, their shortage makes one feel tired or short of breath.
Speak to a Specialist About Copay Assistance
Normally, red blood cells have an average lifespan of 120 days. In autoimmune hemolytic anemia (AIHA), your body’s immune system mistakes red blood cells for unwanted substances, and it attacks the red blood cells and destroys them. As a result, your red blood cells die early. In severe cases, the red blood cells may exist for only a few days.
What Are the Types of Autoimmune Hemolytic Anemia (AIHA)?
Autoimmune hemolytic anemia (AIHA) is classified in 2 ways: Warm vs. cold and primary vs. secondary.
The warm and cold classification of AIHA depends on the antibody involved:
- Warm AIHA: This type of anemia happens at or above normal body temperature. It involves IgG antibodies and is the most common type.
- Cold AIHA: This type of anemia happens in the presence of IgM autoantibodies. This type of anemia happens when you are exposed to cold.
AIHA can also be classified as follows:
- Primary AIHA: AIHA is classified as primary if it develops without any presence of an underlying condition.
- Secondary AIHA: AIHA is classified as secondary if it is linked to an underlying condition like other autoimmune disorders, cancer, or viral infections.
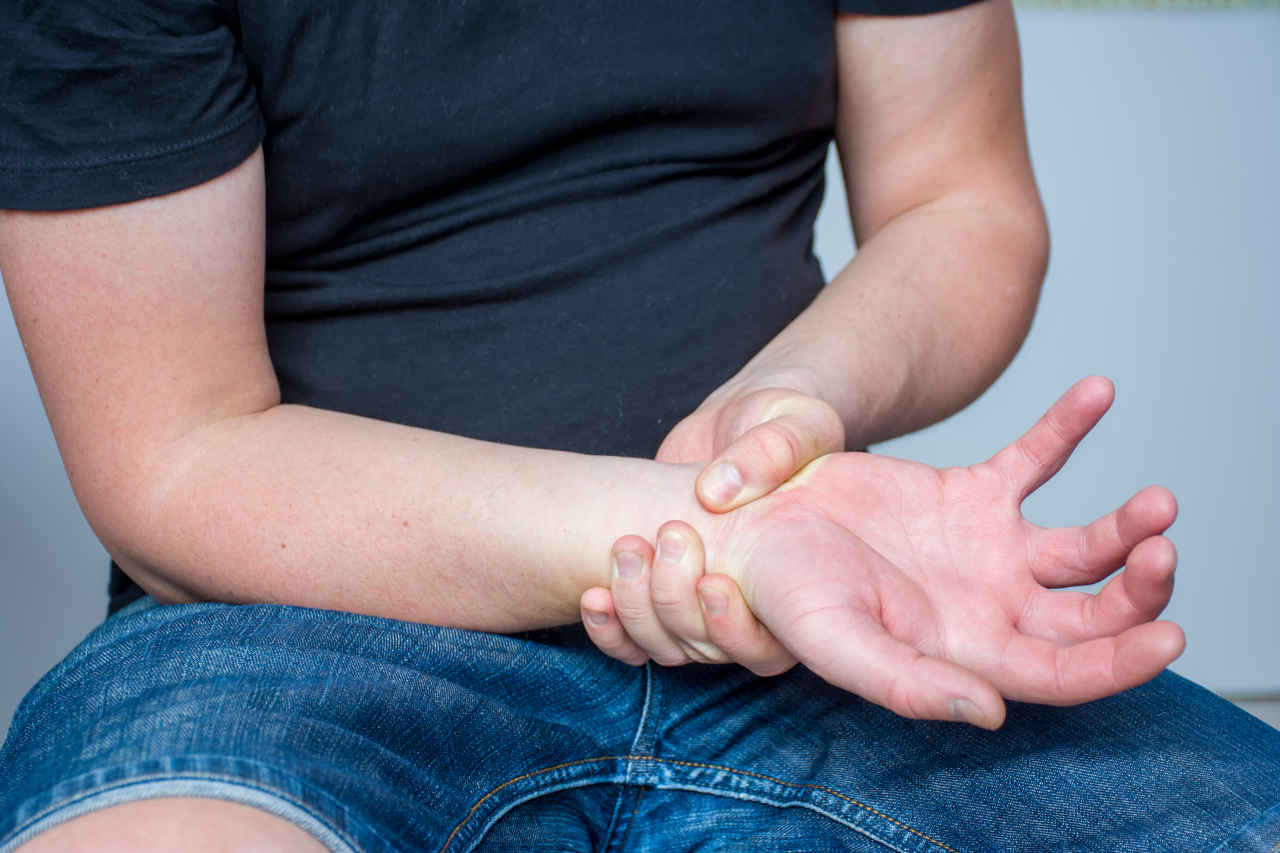
Symptoms

Autoimmune hemolytic anemia (AIHA) is a condition where the body’s own immune system attacks and destroys red blood cells. AIHA can have many signs and symptoms. Some common symptoms of AIHA include:
- Weakness
- Difficulty breathing
- Dark urine
- Thinking and concentration difficulties
- Fever
- Rapid heartbeat
- Jaundice (yellowing of skin or whites of eyes)
- Headache
- Muscle pains
- A sore tongue
What Causes Autoimmune Hemolytic Anemia (AIHA)?
In approximately half of the cases, the exact cause of autoimmune hemolytic anemia (AIHA) is unknown. In other cases, links can be found between AIHA and some other conditions. There could be several factors and disease states that may contribute to the development of AIHA. These include:
Underlying Autoimmune Disorders: Several autoimmune diseases can contribute to the development of AIHA. Some of them include lupus, autoimmune thyroid disease, ulcerative colitis, and rheumatoid arthritis. In these cases, the immune system may produce antibodies that not only target the cells of the associated autoimmune disorder but also attack red blood cells.
Viral Infection: Some viral infections can cause AIHA. These include measles, hepatitis, mumps, epstein-barr virus, and rubella. However, once the infection is treated, the anemia goes away.
Genetics: Parents can pass the gene for the condition on to their children [2].
Medications: In rare situations, certain drugs can trigger immune system responses that result in AIHA. These drugs can include NSAIDS (nonsteroidal anti-inflammatory drugs), anti-cancer drugs, methyldopa, quinidine, and certain antibiotics [1].
Diagnosis
The diagnosis process of AIHA begins with examining the clinical history of the patient. A doctor will identify symptoms related to anemia. After that, the doctor will suggest some tests to confirm AIHA. These tests are:
- Complete Blood Count (CBC): A CBC reveals a low red blood cell count (anemia) in AIHA. Also, it can show increased reticulocyte count, which indicates increased red blood cell production in the body, and the size of the red blood cells the body is making.
- Peripheral Smear: In this test, a healthcare professional examines your blood sample under a microscope to see if your blood cells are being destroyed.
- Coombs Test: This test detects the presence of antibodies that target red blood cells. This test can also tell if anyone has warm AIHA or cold AIHA.
- Lactate Dehydrogenase (LDH): Lactate dehydrogenase is an enzyme found in red blood cells. When red blood cells are damaged, the LDH level increases.
- Cold Agglutinin Titer: If your doctor suspects cold AIHA, he may suggest this test. This test shows the level of the antibody responsible for cold AIHA.
Once diagnosed, your doctor will tailor the treatment plan according to the type and severity of your AIHA and any underlying condition.
Treatment of Autoimmune Hemolytic Anemia (AIHA)
You do not need any treatment if your anemia is mild. It often passes without any treatment. However, in other cases, you may need medications, surgery, or a blood transfusion.
The treatment of autoimmune hemolytic anemia (AIHA) begins with addressing any underlying condition first. If any medication, like penicillin, is causing your anemia, then you have to stop using that medicine. If you have any condition, like lupus or rheumatoid arthritis, that is causing your anemia, then your doctor will treat that condition first.
Here are some common treatment options for autoimmune hemolytic anemia (AIHA):
Medications: The first line of treatment for AIHA is a class of drugs called corticosteroids. They help weaken your body’s immune system and reduce the production of antibodies that target red blood cells. If corticosteroids don’t work, then your doctor may prescribe immunosuppressive medications. Doctors can also prescribe a drug called rituximab. This drug reduces the production of antibodies that target red blood cells [3].
Surgery: If medicines don’t work, then your doctor may recommend surgery to remove your spleen. Your spleen destroys the abnormal red blood cells, including those attached to antibodies. Therefore, the removal of the spleen can decrease your anemia.
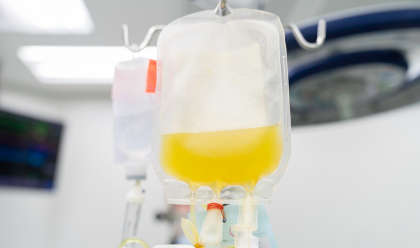
Blood Transfusion: In severe cases, you may need a blood transfusion.
Autoimmune Hemolytic Anemia: FAQs
Here are some common faqs about autoimmune hemolytic anemia:
How Can You Prevent Autoimmune Hemolytic Anemia (AIHA)?
It is not always possible to prevent autoimmune hemolytic anemia (AIHA). This is because, in many cases, we can not determine the exact cause of AIHA. However, if you take medicines that have a link to AIHA, then your doctor may monitor you closely. This will reduce your risk of developing this condition.
How Common Is Autoimmune Hemolytic Anemia?
Autoimmune hemolytic anemia (AIHA) is a rare autoimmune disorder. It only has an annual incidence of 1 – 3 cases per 100,000 people.
What Happens If You Do Not Treat Autoimmune Hemolytic Anemia (AIHA)?
For people with mild AIHA, no treatment is needed. However, treatment is necessary if you have serious anemia. If you do not treat the condition, it can cause heart problems. In severe cases, it can even cause heart failure or death [4].
Who Is Affected Most by Autoimmune Hemolytic Anemia (AIHA)?
Although this disease can happen at any age, people over the age of 40 are most likely to be affected by it. Additionally, females have a greater chance of developing this condition than men [5].
Can AIHA Affect Pregnancy?
During pregnancy, AIHA can cause severe life-threatening anemia in 40 – 50% of cases. It can also cause stillbirth. Also, 35 – 40% of all infants from mothers with AIHA may be born with severe postpartum hemolytic anemia [6].








 Living with TPN at home does not mean you are stuck at home. You can easily manage your nutrition independently or with the help of your caregiver. You can still lead a busy lifestyle. For instance, patients on total parenteral nutrition can still travel for business purposes as well as for social events and vacations. It just takes extra preparation, with guidance and support from your physician or medical team as well as your pharmacist.
Living with TPN at home does not mean you are stuck at home. You can easily manage your nutrition independently or with the help of your caregiver. You can still lead a busy lifestyle. For instance, patients on total parenteral nutrition can still travel for business purposes as well as for social events and vacations. It just takes extra preparation, with guidance and support from your physician or medical team as well as your pharmacist.