Plasmapheresis (or plasma exchange) is a type of intravenous therapy used in severe cases of myasthenia gravis (MG), especially when there is a high risk of respiratory failure. MG is a rare, long-term neurological condition that causes profound muscle weakness and extreme fatigue.
Get Copay Assistance Now
In the United States, around 30,000 to 60,000 people are living with myasthenia gravis. With modern treatments and improved critical care, most people with MG can live a normal or near-normal lifespan. However, severe complications such as myasthenic crisis — which can affect breathing — require urgent medical attention.
There are several treatment options available for MG, but plasmapheresis is one of the fastest-acting and most effective rescue therapies for severe MG symptoms, such as difficulty breathing or swallowing.
If your doctor has recommended plasmapheresis, this article will help you understand what plasmapheresis is, why it is recommended, how the treatment works, what you can expect during the procedure, and its possible benefits and limitations.
Myasthenia Gravis: Brief Overview
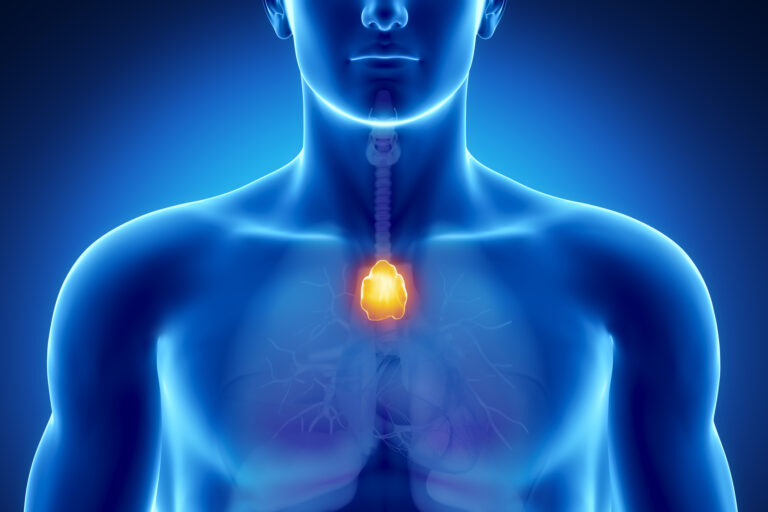
Myasthenia gravis, or MG, is an antibody-mediated autoimmune neurological disorder that affects the voluntary muscles, especially the muscles of the eyes, face, throat, neck, arms, and legs. This condition occurs when the immune system produces autoantibodies that attack the connection between nerves and muscles (known as the neuromuscular junction).
This immune attack makes it harder for muscles to receive signals from the nerves, so they become weak and tire easily. Common symptoms of MG include:
- Drooping eyelids
- Double or blurred vision
- Trouble speaking or swallowing
- General muscle weakness
In severe cases, the weakness can involve the respiratory muscles. This medical emergency, known as a myasthenic crisis, is life-threatening and requires urgent medical care. During a crisis, a person may struggle to breathe, have difficulty speaking clearly, or be unable to swallow food or liquids safely.
While there is no cure for MG, certain treatments, such as oral medications (e.g., corticosteroids, immunosuppressants, cholinesterase inhibitors), surgery (e.g., thymectomy), and intravenous therapy (e.g., IVIG and plasmapheresis), can help manage symptoms and reduce immune activity in patients.
Plasmapheresis: A Form of Treatment for Myasthenia Gravis
Plasmapheresis, or therapeutic plasma exchange (TPE), is a medical procedure in which the liquid part of the blood (plasma) is removed and replaced.
Your blood is made up of four main components: red blood cells, white blood cells, platelets, and plasma. Plasma is the liquid portion that generally contains proteins, antibodies, hormones, and other substances.
In patients with myasthenia gravis (MG), harmful antibodies that attack the neuromuscular junction are present in the plasma. By removing these harmful antibodies, plasmapheresis helps alleviate symptoms, provides rapid symptom relief, and improves muscle strength and motor performance in MG patients.
When It Is Recommended
Doctors recommend plasmapheresis to MG patients under the following circumstances:
- Myasthenic crisis, when breathing or swallowing muscles are severely weakened
- Severe symptom flare-ups, even if a full crisis hasn’t developed
- Before surgery (including thymectomy) to reduce the risk of complications
- When medications are not working well enough or take too long to show benefit
Many MG patients experience rapid symptom improvement within a few days of receiving plasmapheresis.
Speak to a Specialist
About Copay AssistancePlasmapheresis and Myasthenia Gravis: Key Research Insights

Research shows that plasmapheresis can be an effective treatment for people with moderate to severe myasthenia gravis, especially during sudden worsening of symptoms or a myasthenic crisis.
In fact, a real-world study found that plasmapheresis produced rapid clinical improvement in approximately two-thirds (66.7%) of patients with acetylcholine receptor antibody (AChR-Ab)–positive generalized myasthenia gravis. The most notable benefit was improvement in respiratory and limb muscle weakness during disease exacerbations or myasthenic crisis. This study also suggests that plasmapheresis treatment was most effective in patients with higher antibody levels and those with thymus involvement.
Similarly, another study found that people with moderate-to-severe myasthenia gravis showed clear improvement within 2 weeks of plasmapheresis. Patients who had more severe symptoms at baseline, tested positive for acetylcholine receptor antibodies, and had thymic abnormalities or a history of thymectomy were more likely to experience significant benefit.
These findings suggest that certain clinical features can help predict who will respond best to plasmapheresis.
What To Expect During Plasmapheresis
The plasmapheresis procedure is only performed in a hospital or specialized treatment centers. It usually takes 2 to 3 hours, depending on your height, weight, and blood health.
During the treatment:
- You will sit in a reclining chair or lie on a bed.
- A healthcare provider will insert a needle or catheter into your vein (usually in the arm) to draw out the blood.
- The needle or catheter is connected to tubing that carries your blood to the plasmapheresis machine.
- The blood will then slowly pass through a machine to separate the plasma from the blood cells (red cells, white cells, and platelets).
- The plasma, which may contain harmful antibodies, is removed and discarded.
- The remaining blood cells are mixed with a replacement fluid, such as a protein-albumin solution or plasma collected from healthy donors, before they are returned to the body.
- This cycle is repeated until the required volume of plasma is exchanged (usually 1–1.5 times your total plasma volume per session).
You may receive multiple sessions (often four to six sessions) over 1 to 2 weeks, depending on your symptom severity and how well you respond.
Get Financial Assistance
Benefits of Plasmapheresis
Plasmapheresis offers several benefits to MG patients, which include:
1. Rapid Symptom Relief
Unlike many MG medications that take time to resolve symptoms, plasmapheresis removes harmful antibodies directly and helps reduce symptoms quickly, often within days. Patients with severe weakness or breathing problems (myasthenic crisis) benefit the most.
2. Short-Term Treatment
For patients who cannot tolerate high doses of steroids or other immunosuppressive drugs, or who experience other complications, plasmapheresis can be a useful short-term treatment, as it does not rely on immune suppression over the long term.
3. Improved Daily Function and Quality of Life
Plasmapheresis strengthens muscles and improves motor performance. This makes everyday activities like breathing, eating, speaking, and performing routine tasks safer and easier for MG patients.
Side Effects and Limitations of Plasmapheresis
Generally, plasmapheresis is a very safe procedure, but it also has some side effects and limitations.
Possible Side Effects
Serious side effects are rare, but you may feel cold (hypothermic), dizzy, or nauseous during or after the treatment. Hypotension (low blood pressure) and hypocalcemia or hypomagnesemia (low calcium) are also common.
Tell your healthcare provider or medical staff immediately if you experience any of the above side effects.
Limitations
A major limitation is that plasmapheresis provides temporary relief from severe MG symptoms. Because the body continues to produce antibodies, symptoms may gradually return weeks after treatment. For ongoing disease control, doctors rely on medications like immunosuppressants and acetylcholinesterase inhibitors.
Hence, plasmapheresis cannot be used as a long-term standalone treatment for myasthenia gravis. Moreover, if it is used repeatedly, it may increase the risk of serious infections such as catheter-related infections.
Key Takeaway
Plasmapheresis is an effective and widely recommended treatment for providing rapid symptom relief during a myasthenic crisis. However, it does not replace your regular MG medications. Even after plasmapheresis, you will usually need to continue your regular MG medications, such as immunosuppressants or acetylcholinesterase inhibitors, to help control the disease and prevent future flare-ups.
REFERENCES:
- Ipe, T. S., Davis, A. R., & Raval, J. S. (2021). Therapeutic Plasma Exchange in Myasthenia Gravis: A Systematic Literature Review and Meta-Analysis of Comparative Evidence. Frontiers in Neurology, 12, 662856. https://doi.org/10.3389/fneur.2021.662856
- Dresser, L., Wlodarski, R., Rezania, K., & Soliven, B. (2021). Myasthenia gravis: epidemiology, pathophysiology, and clinical manifestations. Journal of Clinical Medicine, 10(11), 2235. https://doi.org/10.3390/jcm10112235
- Sergent, S. R., & Ashurst, J. V. (2023, July 10). Plasmapheresis. StatPearls – NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK560566/
- Bhavaraju-Sanka, R., Jacobs, J., Barthol, C., & Mata, E. (2025). Intravenous immunoglobulin versus plasmapheresis in patients admitted for myasthenic Crisis-Single Hospital Experience (P1-11.031). Neurology, 104(7_Supplement_1). https://doi.org/10.1212/wnl.0000000000211660
- Chen, J., Feng, L., Li, S., Wang, H., Huang, X., Shen, C., & Feng, H. (2024). Therapeutic plasma exchange in ACHR-AB positive generalized myasthenia gravis: a real world study about its early response. Journal of Inflammation Research, Volume 17, 2299–2308. https://doi.org/10.2147/jir.s455104
- Kalita, J., Gutti, N. B., Ahamed, F., Mahajan, R., & Singh, V. K. (2025). Effect of intravenous immunoglobulin or plasmapheresis in myasthenic crisis and worsening myasthenia gravis compared to without rescue treatment. Clinical Therapeutics, 47(9), e1–e6. https://doi.org/10.1016/j.clinthera.2025.06.012
- Carandina-Maffeis, R., Nucci, A., Marques, J. F., Jr, Roveri, E. G., Pfeilsticker, B. H., Garibaldi, S. G., & De Deus-Silva, L. (2004). Plasmapheresis in the treatment of myasthenia gravis: retrospective study of 26 patients. Arquivos De Neuro-Psiquiatria, 62(2b), 391–395. https://doi.org/10.1590/s0004-282×2004000300003
- Bril, V., & Saedi, E. (2025). Rescue therapy in myasthenia gravis. In International review of neurobiology (Vol. 183, pp. 113–132). https://doi.org/10.1016/bs.irn.2025.04.018
- Kumar, R., Birinder, S. P., Gupta, S., Singh, G., & Kaur, A. (2014). Therapeutic plasma exchange in the treatment of myasthenia gravis. Indian Journal of Critical Care Medicine : Peer-Reviewed, Official Publication of Indian Society of Critical Care Medicine, 19(1), 9. https://doi.org/10.4103/0972-5229.148631