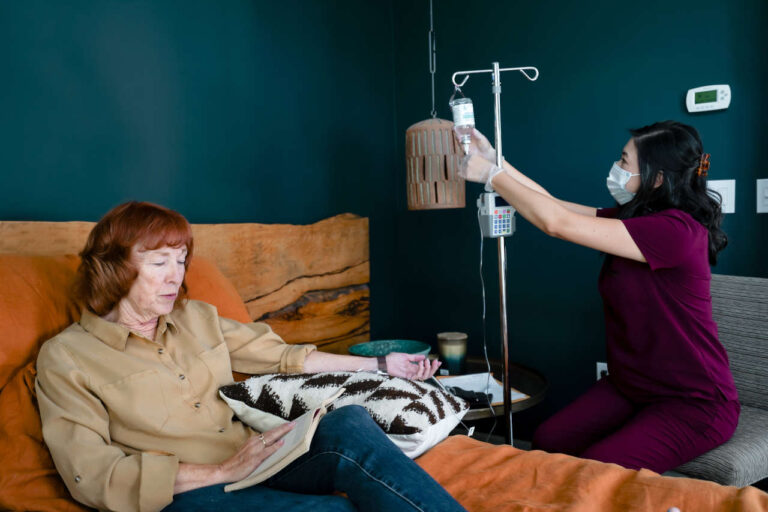
Immunoglobulins (Ig) were initially identified in our blood as “neutralizing substances.” These substances were found effective to counteract infections, such as Corynebacterium diphtheria. They were discovered in 1890 by two immunologists, Emil von Behring and Kitasato Shibasaburo.
Immunoglobulins constitute roughly 20% of protein in our blood. Immunoglobulins are special types of proteins that have a carbohydrate group attached to their chain (scientifically known as glycoproteins). These glycoproteins play an important role in maintaining the body’s immune system. The term immunoglobulins is interchangeable with the term, antibodies.
Immunoglobulins are highly specific and secreted in massive amounts by plasma cells in response to disease-causing toxins or substances (pathogenic antigens) being introduced to the body.
Key Takeaways
- There are 5 types of immunoglobulins: IgG, IgM, IgA, IgD, and IgE.
- IgG is the most common type, making up roughly 75% of antibodies in the blood.
- IgM is the first antibody produced in response to a new infection.
- IgA is the primary antibody found in saliva, tears, and breast milk.
- Low immunoglobulin levels can indicate primary immunodeficiency or autoimmune disease.
- IVIG therapy uses pooled immunoglobulins to treat conditions like primary immunodeficiency, Guillain-Barre syndrome, and myasthenia gravis.
What Are the Functions of Immunoglobulins?
Immunoglobulins protect us against:
- Bacteria
- Chemical substances
- Viruses
- Parasites
- Allergens
- Synthetic substances
- Cancerous cells
- Fungus
Speak to a Specialist
About IV Immunoglobin TherapyPlasma cells produce specific antibodies against a particular antigen.
For instance, antibodies released by plasma cells against the COVID-19 virus will only bind to the COVID-19 virus and not any other virus or bacteria. This specificity of different immunoglobulin types makes the body’s immune system more active against multiple pathogenic invasions.
Body Fluids That Contain Immunoglobulins:
- Breast milk
- Tears
- Saliva
- Gastric secretions
- Mucosal secretions
The primary function of different types of Ig is to produce an antibody-mediated response by binding to the foreign antigen. The antibody-mediated humoral immune response kills the invading microbes and prevents infections from spreading to other parts.
There are five different types of immunoglobulins (IgG, IgM, IgA, IgD, and IgE). Each vary based on their functions, chemical structure, biological features, distribution, and target specificity.
Any genetic abnormality detected in our bodies during antibody processing or any variation in the normal immunoglobulin levels will increase the risk of developing various immunological diseases. These immunological responses may include primary immune deficiency diseases or autoimmune diseases (a condition in which immune cells attack the healthy cells of the body).
Medical researchers have taken advantage of different immunoglobulin types and their functions to treat various disorders. For example, gamma globulins (a major immunoglobulin) are used as immunotherapy for treating multiple viral infections, bacterial infections, and autoimmune disorders associated with humoral immune deficiency.
Basic Structure of Immunoglobulins
Immunoglobulins are Y-shaped globular proteins about 10 nm in size and 150kDa in molecular weight.
All immunoglobulins consist of four common polypeptide subunits:
- Two identical heavy chains.
- Two identical light chains.
The polypeptide chains represent different types of Ig that are held together with a disulfide bridge and form a Y-shaped structure.
This Y-shaped structure is divided into two regions:
- The bottom part is called a constant region.
- The upper, two-arm part is called a variable region.
As the name implies, the constant region does not change from one immunoglobulin type to another, but the variable region does.
Furthermore, the variable region of the antibody, called the fragment of antigen-binding (Fab) site, binds to specific antigens.
The region of the antigen that binds to the antigen-binding site is called an epitope.
The constant region is typically the tail of the antibody called the fragment of crystallization (Fc). It binds to the surface of immune cells or interacts with receptor proteins of the complement system.
All immunoglobulin types exhibit dual functionality: binding to viruses or bacteria and mediating biological immune responses such as complement system activation, opsonization, and neutralization of microbial toxins and viruses.
Safe IVIG Administration
Immunoglobulins Mechanism of Action
Immunoglobulins work to protect the body’s immune system by regulating the multiple cell destruction pathways, each depending on the type of signals they receive or the pathogens they interact with.
Immunoglobulins are generally present either on the surface of B-cells or circulating freely in body fluids. The binding of the antibody to its specific antigen results in the formation of an antibody-antigen complex which elicits an immune response.
The immunoglobulins kill off the foreign invaders through three mechanisms:
- Neutralization
- Opsonization
- Complement activation
Neutralization
The neutralization mechanism focuses on inactivating foreign material or bacteria. When the antibody binds to the functional part of the virus or bacteria, it inactivates the virus’ ability to attach to the surface of healthy cells. As a result, the biological effect of the toxins released by bacteria and viruses is neutralized.
Opsonization
In opsonization, antibodies recognize and label the infected or cancerous cells. The labeled cells are then digested and removed by phagocytic cells such as macrophages or cytotoxic T-cells. As a result, the opsonization pathway enhances phagocytosis.
Activation of the Complement System
The binding of immunoglobulins to pathogens leads to the activation of complement proteins. Upon activation, these proteins build a membrane attack complex (MAC). The MAC proteins then cause the cell to burst (lysis) by punching holes in the cell membrane of the bacteria. Different types of Ig ⏤ IgG and IgM antibodies ⏤ are effective in activating the complement pathways.
Immunoglobulin Types and Their Functions
The human body only makes five types of immunoglobulins:
- IgG
- IgM
- IgA
- IgD
- IgE
These immunoglobulins protect the body from multiple types of antigens. All antibodies differ based on their amino acid sequence in the constant region, structure (monomer, pentamer, and dimer), short life in the blood, site, and immunological properties.
Quick Comparison of the 5 Types of Immunoglobulins:
| Type | % of Serum Antibodies | Half-Life | Primary Location / Role |
| IgG | 70-75% | ~21 days | Blood, tissue; long-term immunity, crosses placenta |
| IgM | 5–10% | ~5 days | Blood; first responder to new infections |
| IgA | 10–15% | ~6 days | Mucous membranes, secretions (saliva, tears, breast milk); provides barrier protection |
| IgD | <0.5% | ~3 days | B-cell surface; signal receptor for B-cells |
| IgE | <0.01% | ~2 days | Mast cells, basophils; allergy and antiparasitic response |
Get IVIG Prior Authorization
Immunoglobulins G (IgG)
- Immunoglobulin G (IgG) is the most common and abundant antibody present in the body.
- Blood plasma consists of 75-80% of IgG antibodies.
- Of all immunoglobulin types, IgG has the longest lifespan of about 23 days.
- IgG is the only antibody that can cross the placental barrier and provide passive immunity to a developing fetus.
IgG antibodies remember the pathogens that have previously entered the body and caused an infection. IgG also provides some immunity to infants when ingested through breast milk.
These types of Ig enhance the elimination of pathogens, neutralize bacterial or viral toxins, and trigger the activation of the complement system.
IgG has four isotype classes:
- IgG1
- IgG2
- IgG3
- IgG4
Immunoglobulin M (IgM)
Immunoglobulin M (IgM) is the first antibody that interacts with new bacteria that enter the body and initiates a primary immune response.
IgM is also called a natural antibody because it serves as the first line of defense of the immune system and provides short-term protection.
These types of Ig have a gigantic pentamer structure above all other antibodies and consist of 10 antigen-binding sites, making them more effective than IgG in killing bacteria or viruses.
The life span of the IgM antibody in our body is about five days. These immunoglobulin types make up 5% – 10% of the antibodies in blood plasma.
IgM also causes formation of clumps (agglutination) of bacteria when binding to the epitope surface. The IgM antibody is a potent agglutinin. It also exists in its monomeric form on the surface of naïve B-cells and red blood cells.
Immunoglobulins A (IgA)
Immunoglobulin A (IgA) is the most common antibody following IgG. This type of immunoglobulin is present in the blood, lymph, and other body secretions such as saliva, tears, and milk. It can also be found in the genital lining, respiratory tract, and intestine lining.
IgA antibodies protect the body from bacterial growth and colonization. However, it is less stable than IgG and found in a lower quantity, accounting for about 10% – 15% of the total immunoglobulins in the blood.
These types of Ig are often called secretory antibodies. Primarily, due to the attached secretory component found on their structure. This component protects them from degradation through enzymatic digestion. On average, an individual secretes about 5g to 15g of secretory IgA into mucous secretions each day to prevent disease or disorder development (pathogenesis).
Immunoglobulins D (IgD)
Immunoglobulin D (IgD) makes up less than 0.5% of serum antibodies. This type of immunoglobulin is found in smaller amounts within lymphatic fluids and blood.
The function of IgD is still unknown, but it is present on the surface of immature B-cells and works as the surface to receive a signal (receptors). It is also a part of the innate immune system. Researchers believe that IgD regulates the B-cells’ activation and differentiation into plasma cells.
Get IVIG Copay Assistance
Immunoglobulins E (IgE)
Immunoglobulin E (IgE) makes up less than 0.01% of serum antibodies. Even though it is present in the lowest amount in the blood and has a shorter lifespan, it is still a potent antibody.
This immunoglobulin type is the most effective antibody against parasitic infections, including helminths.
A high level of IgE in the blood can sometimes cause hypersensitivity toward non-harmful substances such as pollen or dust particles. Recently, immunologists have begun formulating new anti-IgE antibodies for treating allergies and asthma.

Which Type of Immunoglobulin Is Present in Tears, Saliva, and Breast Milk?
Antibodies found in breast milk are IgA, IgE, IgM, IgD, and IgG, with the highest levels of IgA found in the first milk a mother produces during pregnancy (colostrum). Up to 50% of proteins in breast milk colostrum are due to the presence of IgA. This type of immunoglobulin can also be found in tears and saliva.
IgA antibodies have two sub-classes: IgA1 and IgA2. Each contributes to its own biological properties.
Diseases Related to Immunoglobulin Deficiency
Immunologists have identified that a person could have an immunoglobulin deficiency or non-functional immunoglobulins due to a defective immune system. This rare genetic condition is known as primary immunodeficiency disease (PIDD).
Medical researchers have already reported more than 300 types of primary immunodeficiency diseases.
In addition, some secondary immunodeficiency disorders are caused by external environmental factors such as:
- Severe malnutrition
- HIV
- Chemotherapeutic agents
People suffering from primary immunodeficiency disease are likely to have weaker immune systems. Therefore, they are more prone to infections and other severe immunological problems.
Get IVIG Copay Assistance
Speak to a SpecialistImmunoglobulins Blood Test and Their Indications
People who suffer from common infections and/or recurrent diseases at repeated intervals may have a weakened immune system.
This could be due to their low levels of immunoglobulins (immunity) that are needed to fight off diseases. In these instances, medical professionals highly recommend an immunoglobulin blood test.
An immunoglobulin blood test is conducted by taking a small blood sample from the patient’s body to estimate the level of specific antibodies such as IgA, IgG, and IgM. Ig tests help diagnose various health problems that affect different immunoglobulin types and their functions in the body.
The antibody results are measured by comparing them with the normal immunoglobulin range. If IgA, IgG, and IgM levels are too high or low, there is an increased risk of severe health problems.
High IgG Levels May Indicate the Presence Of:
- HIV/AIDS
- Long-term hepatitis
- Multiple sclerosis
- Multiple myeloma
Low IgG Levels May Indicate the Presence Of:
- X-linked agammaglobulinemia disease
- Leukemia
- Nephritic syndrome
The causes of this type of immunoglobulin deficiency are still unknown, but it could occur due to genetic defects.
High IgA Levels Indicate the Presence of Autoimmune Disorders Such As:
- Chronic hepatitis
- Systemic lupus erythematosus (SLE)
- Cirrhosis
- Multiple myeloma
- Rheumatoid arthritis
Low IgA Levels Increase the Risk Of:
- Autoimmune diseases
- Enteropathy
- Kidney damage
Some people are born with an IgA deficiency or a defective gene that produces too little IgA in the body.
High IgM Levels May Indicate the Presence Of:
- Early viral hepatitis
- Kidney damage
- Rheumatoid arthritis
This type of Ig serves as the first line of defense. A rise in the IgM levels in the blood indicates that the body has been exposed to new infections.
People suffering from inherited immune diseases such as leukemia or multiple myeloma are more likely to have low levels of this immunoglobulin type in their blood.
Get At-Home IVIG Infusion
Common Symptoms of IgA, IgM, and IgG Deficiency:
- Bronchitis
- Pneumonia
- Respiratory infections
- Gastrointestinal infections
- Frequent fever
- Skin allergies
- Sinus and lung infections
- Unexplained weight loss
- Diarrhea
Other Related Conditions:
- Kawasaki disease
- Organ transplantation
- Severe combined immunodeficiency disorders (SCID)
- And many others
Early symptoms and diseases can vary from person to person.
Get IVIG Copay Assistance
IVIG Financial AssistanceClinical Use of Immunoglobulins
Introducing different immunoglobulin types and their functions is recognized as the most effective immunotherapy to treat infectious and primary immunodeficiency disorders.
Immunoglobulin replacement therapy was initially introduced in 1952. It was used as a treatment for X-linked agammaglobulinemia (a genetically inherited condition). Over the past three decades, it has become the standard method for treating PIDD.
The primary goal of Ig replacement therapy is to provide strong immunity, stop invasive bacterial infections, and enhance the patient’s survival rate. Recent advancements in Ig replacement therapy have substantially shown to improve the quality of life for many patients with PI disorders.
Routes of IVIG Administration

There are two main routes of administration for Ig replacement therapy:
- Subcutaneously (SCIG)
- Intravenously (IVIG)
There are several important factors to take into account when determining the administration route for a patient. These may include the patient’s preference, previous medical history, IV access, cost, availability, and tolerability.
Subcutaneous Immunoglobulin Therapy (SCIG)
SCIG injection is given into the fatty (subcutaneous) layer of the skin. It is injected through slow diffusion in small doses using a fine needle which is placed at different sites, such as the abdomen, thigh, or upper arm.
The average volume of SCIG injection is between 10 ml to 25 ml, with repeated intervals of once or twice a week.
SCIG injections generally take 1 to 2 hours to complete and can be self-administered at home with a mechanical infusion pump.
Choosing the correct size and number of needles for this type of immunoglobulin therapy is crucial to ensure a successful injection.
Intravenous Immunoglobulin Therapy (IVIG)
IVIG is directly administered through a vein in larger volumes and takes approximately 2 to 6 hours to complete.
On average, repeated doses are given every 3 to 4 weeks.
The dose and frequency of IVIG depend on the patient’s current body weight and disease state. The estimated starting dosage is 2 g/kg/month divided over 4 to 5 days.
Uses of Immunoglobulin Therapy
Different immunoglobulin types and their functions are used to treat various conditions, which include some, but are not limited to the following
- Primary immunodeficiency
- Chronic inflammatory demyelinating polyneuropathy
- Immune thrombocytopenic purpura
- Myasthenia gravis
- Lupus, myositis, multiple sclerosis
- Guillain-Barre syndrome
- Stiff man syndrome
- Bone marrow transplantation
- Kawasaki disease or other neurological disorders
Can IVIG help?
Free IVIG Treatment Info | Difficulty In Diagnosing?Common and Adverse Side Effects
Common Side Effects:
- Headache
- Body ache
- Nausea
- Diarrhea
- Muscle cramps
Adverse Side Effects:
- Severe allergic reactions:
- Hives
- Swelling in mouth, face, or throat
- Wheezing or trouble breathing
- Kidney problems
- Blood clots
- Aseptic meningitis syndrome
- Hemolysis (destruction of red blood cells)
- Transfusion-related acute lung injury
Side effects experienced by patients are often due to fast infusion rates and product temperatures.
To prevent or alleviate these side effects:
- Patients should be fully hydrated before receiving an infusion.
- Product should be brought to room temperature prior to administration.
- Pre-medications may be given prior to the infusion, such as diphenhydramine, acetaminophen, corticosteroids, or non-steroidal anti-inflammatory drugs.
- The IVIG infusion rate should be titrated in 30-minute increments.
- A trained nurse should monitor vital signs throughout the infusion.
Frequently Asked Questions
What are the 5 types of immunoglobulins?
The five types of immunoglobulins are IgG, IgM, IgA, IgD, and IgE. IgG is the most abundant, making up 70-75% of total serum antibodies and providing long-term immunity. IgM is the first antibody produced in response to a new infection. IgA is the primary antibody in saliva, tears, and breast milk. IgD functions mainly as a B-cell surface receptor. IgE is involved in allergic reactions and antiparasitic immunity.
What is the most common type of immunoglobulin?
IgG is the most common type of immunoglobulin. It makes up 70-75% of the antibodies found in blood plasma and has the longest half-life of all immunoglobulin types, at approximately 21 days. IgG is the only immunoglobulin that can cross the placental barrier, providing passive immunity to the developing fetus.
What happens if your immunoglobulins are low?
Low immunoglobulin levels can indicate a primary immunodeficiency disease (PIDD), such as X-linked agammaglobulinemia, or a secondary immunodeficiency caused by factors like HIV, malnutrition, or certain medications. Common symptoms of immunoglobulin deficiency include recurrent infections (respiratory, gastrointestinal), frequent fever, skin allergies, and unexplained weight loss. An immunoglobulin blood test can confirm deficiency, and IVIG or SCIG therapy may be used to replace missing antibodies.
What is IgM, IgG, IgA, IgD, and IgE?
These are the five classes (isotypes) of immunoglobulins, also called antibodies. IgM is the first-responder antibody and acts as the initial line of defense. IgG provides long-term immunity and is the most abundant. IgA protects mucosal surfaces such as the gut, lungs, and secretions. IgD is found mainly on the surface of B-cells and helps regulate immune activation. IgE is present in small amounts but plays a key role in allergic reactions and defense against parasites.
What are the 4 subtypes of IgG?
IgG has four isotype subclasses: IgG1, IgG2, IgG3, and IgG4. Each subclass has slightly different structural properties and plays a different role in the immune response. IgG1 and IgG3 are the most effective at activating the complement system. IgG4 is often associated with allergic and inflammatory conditions. The specific subclass can affect how the immune system responds to different types of antigens.
What do immunoglobulins do?
Immunoglobulins (antibodies) protect the body against pathogens including bacteria, viruses, fungi, and parasites. They work through three main mechanisms: neutralization (blocking the ability of a pathogen to infect cells), opsonization (tagging pathogens for destruction by immune cells), and complement activation (triggering a cascade that destroys bacteria by punching holes in their membranes). Different immunoglobulin types specialize in different parts of the immune response.
REFERENCES:
- Schroeder Jr, H. W., & Cavacini, L. (2010). Structure and function of immunoglobulins. Journal of Allergy and Clinical Immunology, 125(2), S41-S52.
- Janeway Jr, C. A., Travers, P., Walport, M., & Shlomchik, M. J. (2001). The structure of a typical antibody molecule. In Immunobiology: The Immune System in Health and Disease. 5th edition. Garland Science.
- Vaillant, A. A. J. (2021). Immunoglobulin. StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK513460/.
- Introduction to Immunoglobulins. Thermo Fisher Scientific – US. (n.d.). https://www.thermofisher.com/pk/en/home/life-science/antibodies/antibodies-learning-center/antibodies-resource-library/antibody-methods/introduction-immunoglobulins.html
- Encyclopædia Britannica, inc. (n.d.). Classes of immunoglobulins. Encyclopædia Britannica. https://www.britannica.com/science/immune-system/Classes-of-immunoglobulins#ref215568.
- Intravenous Immunoglobulin (IVIG). rheumatology.org. (n.d.). https://www.rheumatology.org/I-Am-A/Patient-Caregiver/Treatments/Intravenous-Immunoglobulin-IVIG.
- Jolles, S., Sewell, W. A. C., & Misbah, S. A. (2005). Clinical uses of intravenous immunoglobulin. Clinical and experimental immunology, 142(1), 1.
- Sriaroon, P., & Ballow, M. (2015). Immunoglobulin replacement therapy for primary immunodeficiency. Immunology and Allergy Clinics, 35(4), 713-730.
- http://www.igliving.com/magazine/articles/IGL_2009-10_AR_Choosing-Needles-for-IVIG-and-SCIG.pdf