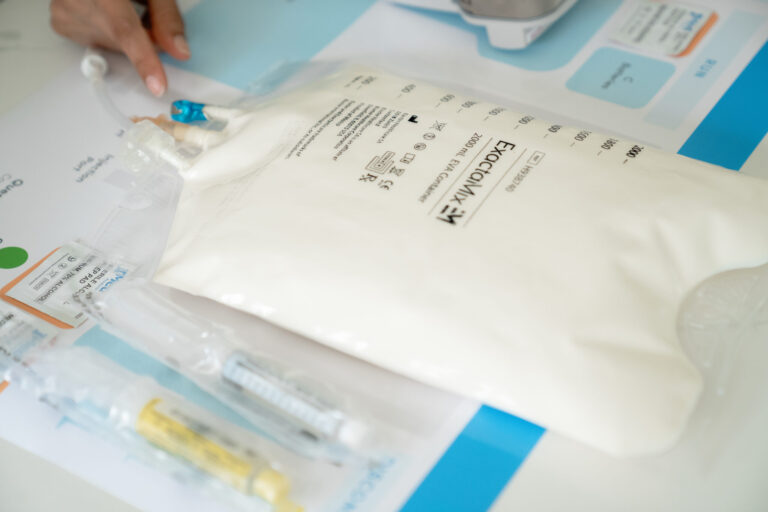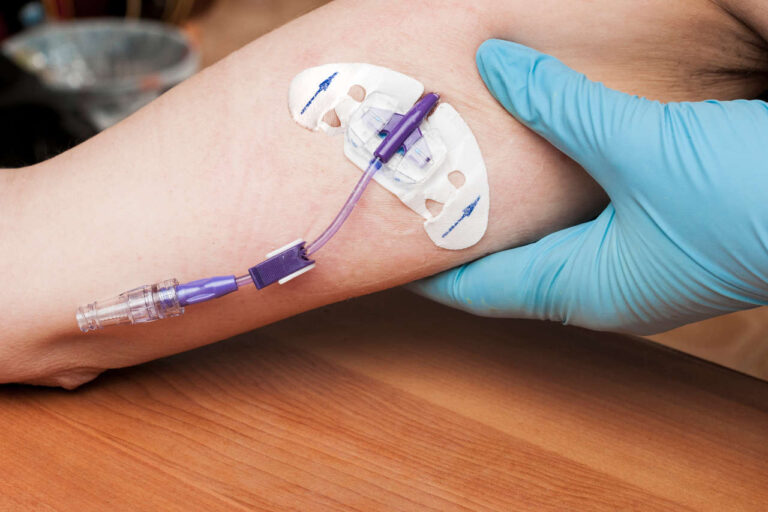
Total parenteral nutrition (TPN), commonly known as intravenous feeding, is typically recommended by doctors to cancer patients to fulfill their nutritional requirements. It is given under certain conditions, such as when tube feeding is not feasible, or patients experience gastrointestinal toxicity/dysfunction due to cancer that limits oral intake. Cancer and its treatments not only affect the patient’s body but also disrupts their ability to eat and absorb essential nutrients, putting them at high risk of malnutrition (a condition when a body does not receive essential nutrients).
IV Fluids Fully in Stock
Consistent availability, uninterrupted careMalnutrition is one of the most prevalent concerns among cancer patients that adversely affects the quality of life and survival of these patients. It’s been estimated that up to 20% of oncology patients die from the detrimental effects of malnutrition rather than the malignancy itself.
In this article, we will discuss the importance of TPN for cancer patients, how it benefits individuals fighting cancer, and why it plays a vital role in their treatment and recovery process.
Before addressing the importance of TPN for cancer, let’s first understand why nutrition is important for cancer patients and, conversely, how malnutrition affects them.
Nutrition and Cancer
Just like a healthy individual needs a well-balanced diet to stay strong and resilient, cancer patients also require proper nutrition to support their bodies to fight the disease. Adequate nutrition is important for cancer patients because:
- It supports the immune system
- It provides energy and strength
- It aids in tissue repair and healing
- It enhances treatment tolerance and effectiveness
- It prevents malnutrition and weight loss
- It improves the quality of life and supports emotional well-being
By maintaining nutritional needs, cancer patients can optimize their treatment outcomes, maintain a better quality of life, and enhance their overall well-being.
How Nutrient Deficiency or Malnutrition Occurs in Cancer Patients
Malnutrition in cancer patients can arise from various factors related to the disease itself and its treatments. For instance, anticancer treatments like high-dose chemotherapy, radiation therapy, and bone marrow transplantation often present side effects that hinder a patient’s ability to eat and absorb nutrients.
Some of the common adverse effects faced by cancer patients during the terminal phase of cancer or anticancer treatments are nausea, vomiting, mouth sores, loss of appetite, and difficulty swallowing. These side effects often result in malnutrition and weight loss. Similarly, in other cases, several surgical procedures or treatments targeting the gastrointestinal tract can also impact nutrient absorption.
When the body does not receive adequate calories, proteins, vitamins, and minerals necessary for optimal functioning and healing, it significantly impacts the body’s ability to fight the disease and heal.
How Malnutrition Affects Cancer Patients
Malnutrition can have severe consequences for cancer patients, affecting their overall health and treatment outcomes. Some of the consequences include:
- Weakened Immune System: Malnutrition compromises the immune system’s ability to fight infections, making cancer patients more susceptible to complications and delaying their recovery.
- Muscle Wasting: Inadequate nutrient intake can lead to muscle wasting (cachexia) in cancer patients, resulting in weakness, fatigue, and reduced functional ability.
- Impaired Wound Healing: Malnutrition hinders the body’s ability to heal wounds, increasing the risk of infections and delaying recovery from surgery or other medical procedures.
- Treatment Toxicity: Malnourished patients may experience increased side effects from cancer treatments due to compromised organ function and reduced tolerance to therapy.
- Reduced Quality of Life: Malnutrition can significantly impact a patient’s quality of life, leading to fatigue, depression, and a diminished sense of well-being.
Prolonged and severe malnutrition can put cancer patients at greater risk for complications associated with cancer treatments. Doctors mostly recommend TPN to improve the nutritional status of cancer patients and prevent malnutrition-associated complications.
Ask About TPN Home Infusion
Importance of TPN for Cancer Patients
TPN is important for cancer patients as it effectively reduces the side effects of anticancer treatments and prevents malnutrition by stabilizing the nutritional state of patients who are unable to meet their nutritional needs through regular oral intake. This nutritional intervention provides a complete and balanced nutritional support system, ensuring that cancer patients receive the necessary macronutrients and micronutrients to support their body’s functions and recovery.
The solution of TPN contains proteins, carbohydrates, fats, vitamins, minerals, and other essential nutrients necessary for cell growth, tissue repair, and overall well-being. The TPN solution is customized to meet the individual nutritional requirements of each patient.
By receiving these nutrients intravenously, cancer patients can maintain their nutritional status and prevent further deterioration due to inadequate oral intake.
Benefits of TPN for Cancer Patients
The utilization of TPN in cancer patients offers several other benefits in preventing malnutrition, such as:
Tissue Repair and Healing
Cancer treatments, such as chemotherapy and radiation therapy, can damage healthy cells along with cancer cells. TPN provides the body with the necessary nutrients for tissue repair and healing to support recovery.
Weight Maintenance and Muscle Preservation
Cancer patients may experience unintentional weight loss and muscle wasting, which can have detrimental effects on their overall health and treatment response. TPN helps maintain adequate calorie and protein intake, prevents further weight loss, and preserves muscle mass.
Support for Immune Function
Cancer and its treatments weaken the immune system, making patients more susceptible to infections. TPN provides immune-boosting nutrients, such as vitamins and minerals, to support immune function and reduce the risk of complications.
Enhancement of Treatment Tolerance
Cancer treatments can cause side effects, and malnutrition can exacerbate these effects, making it difficult for patients to tolerate therapy. By providing optimal nutrition, TPN helps patients better tolerate their treatments and potentially improve treatment outcomes.
Pre- and Post-operative Support
Some cancer patients undergo surgery as part of their treatment plan. TPN may be administered before and after surgery to ensure patients are well-nourished, promote wound healing, and reduce the risk of postoperative complications.
Although TPN is safe and well-tolerated for patients, it also can have a number of risks, such as infection, nutrient overload, hypoglycemia, and electrolyte imbalance. Therefore, it is important to carefully monitor the TPN mixture and maintain a strict sterile technique.
AmeriPharma® Specialty Care
Total Parenteral Nutrition | Leader In TPN AssistanceConclusion
In summary, TPN plays a crucial role in supporting cancer patients who struggle to consume adequate nutrients orally. TPN helps maintain nutritional status, promotes healing, and improves overall well-being by directly delivering essential nourishment into the bloodstream. While TPN also carries some potential risks, they can be reduced by taking appropriate precautions and conducting regular evaluations. Overall, TPN provides vital support and enables cancer patients to focus on their recovery and journey toward better health.
REFERENCES:
- Yan, X., Zhang, S., Jia, J., Yang, J., Song, Y., & Duan, H. (2022). Total Parenteral Nutrition Treatment Improves the Nutrition Status of Gynecological Cancer Patients by Improving Serum Albumin Level. Frontiers in Medicine, 8, 759387. https://doi.org/10.3389/fmed.2021.759387
- Amin, S. B., Livshin, S., & Maheshwari, A. (2017). Parenteral Nutrition in Advanced Cancer. In Diet and Nutrition in Critical Care (pp. 1897–1912). https://doi.org/10.1007/978-1-4614-7836-2_119
- Joque, L., & Jatoi, A. (2005). Total parenteral nutrition in cancer patients: why and when? PubMed, 8(2), 89–92. https://pubmed.ncbi.nlm.nih.gov/16013227
- Copeland, E. M., Pimiento, J. M., & Dudrick, S. J. (2011). Total Parenteral Nutrition and Cancer: From the Beginning. Surgical Clinics of North America, 91(4), 727–736. https://doi.org/10.1016/j.suc.2011.04.003
- Loaiciga, F., & Dev, R. (2018). Parenteral Nutrition in Cancer Patients Undergoing Chemotherapy. https://doi.org/10.1093/med/9780190658618.003.0023
- Akbulut, G. (2011). New perspective for nutritional support of cancer patients: Enteral/parenteral nutrition. Experimental and Therapeutic Medicine, 2(4), 675–684. https://doi.org/10.3892/etm.2011.247
- Hoda, D., Jatoi, A., Burnes, J., Loprinzi, C., & Kelly, D. (2005). Should patients with advanced, incurable cancers ever be sent home with total parenteral nutrition? Cancer, 103(4), 863-868. https://doi.org/10.1002/cncr.20824
- Yan, X., Zhang, S., Jia, J., Yang, J., Song, Y., & Duan, H. (2021). Exploring the malnutrition status and impact of total parenteral nutrition on the outcome of patients with advanced stage ovarian cancer. BMC Cancer, 21(1). https://doi.org/10.1186/s12885-021-08537-6
- Cotogni, P. (2016). Enteral versus parenteral nutrition in cancer patients: evidences and controversies. PubMed, 5(1), 42–49. https://doi.org/10.3978/j.issn.2224-5820.2016.01.05
- Virizuela, J. A., Camblor-Álvarez, M., Luengo-Pérez, L. M., Grande, E., Álvarez-Hernández, J., Sendrós-Madroño, M. J., Capdevila, J., Cervera-Peris, M., & Ocón-Bretón, M. J. (2017). Nutritional support and parenteral nutrition in cancer patients: an expert consensus report. Clinical & Translational Oncology, 20(5), 619–629. https://doi.org/10.1007/s12094-017-1757-4