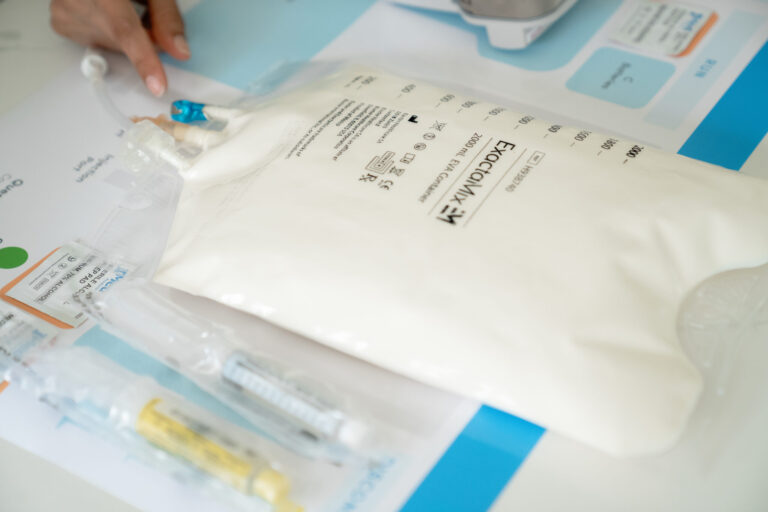
Total parenteral nutrition (TPN), while often regarded as a lifeline for many patients, is not universally suitable. This life-saving technique has several contraindications. The term “contraindication” refers to a situation or state in which a specific treatment or intervention should be avoided because it may be harmful or ineffective for the patient.
IV Fluids Fully in Stock
Consistent availability, uninterrupted careA contraindication is a red flag that alerts healthcare providers to continue with caution or seek alternate options.
As a result, if you or a loved one has chosen to get TPN therapy, you need to be informed of the risks.
The goal of this article is to give readers a thorough grasp of TPN contraindications and to explore the situations or conditions under which TPN therapy should not be administered.
TPN-Associated Contraindications
While TPN serves a crucial purpose in nourishing individuals unable to receive nutrients through their gastrointestinal tract, it’s imperative to understand that this method of nutritional support is not always applicable.
There are specific medical conditions and scenarios where TPN should not be administered. Let’s explore these contraindications one by one:
Infants with Less Than 8 cm of Small Bowel
Babies are incredibly delicate, especially their gastrointestinal systems. TPN may not be suitable for infants with less than 8 cm of small bowel because it bypasses the digestive system entirely. For these tiny patients, enteral feeding, which involves feeding through the stomach or intestines, is often a safer and more effective alternative.
Irreversibly Decerebrate Patients
Decerebrate posturing is a severe neurological condition in which patients exhibit abnormal and rigid postures, typically characterized by extension of the arms and legs. In patients with irreversible decerebrate posturing, TPN may not offer significant benefits, and it’s crucial to focus on palliative care and comfort measures.
Critical Cardiovascular Instability or Metabolic Instabilities
Another crucial contraindication for TPN involves patients with severe cardiovascular instability or metabolic instabilities. TPN administration should be delayed until these concerns are handled and stabilized, as administering TPN in such circumstances may exacerbate pre-existing problems.
When the Patient Is Stable, and Gastrointestinal Feeding Is feasible
TPN is generally reserved for patients who are critically ill or in an unstable condition, rendering them unable to tolerate enteral nutrition. In cases where a patient’s stability allows for gastrointestinal feeding, it is usually the preferred choice over TPN. Gastrointestinal feeding is a more natural, cost-effective, less invasive approach that fosters improved long-term outcomes while reducing the risk of infections.
When Short-Term TPN Suffices
The duration of TPN is an important consideration. Patients may only require TPN for a brief period of time. TPN is an effective treatment, however it is not necessarily the best long-term choice. Complications can arise from long-term TPN without a clear treatment purpose.
Lack of a Therapeutic Goal
In cases where there is no therapeutic goal other than prolonging life in a terminal condition, TPN is not recommended. Its use in such circumstances may not align with the patient’s best interests.
TPN and Severe Infection (Sepsis)
Sepsis is a life-threatening condition where the body’s response to infection can lead to organ failure. TPN can suppress the immune system, which makes it unsuitable for patients battling severe illnesses like sepsis. TPN should not be administered to patients who have active infections since it increases the risk of infection aggravation.
TPN and Liver Diseases
Patients with severe liver diseases may not tolerate TPN well. The liver plays a crucial role in processing nutrients from the bloodstream. TPN is contraindicated in patients with severe liver disorders because it can exacerbate liver dysfunction.
Boxed Warning: TPN and Intravenous Fat Emulsions
The Food and Drug Administration (FDA) has issued a boxed warning concerning certain intravenous fat emulsions utilized in TPN, particularly for preterm neonates. This warning emphasizes the heightened risk of fat accumulation in the lung’s blood vessels, which can lead to an increased risk of mortality. Therefore, healthcare providers must exercise utmost care and adhere to evidence-based guidelines when considering TPN therapy for premature infants.
Get Financial Assistance for TPN
Frequently Asked Questions (FAQs)
Are TPN contraindications absolute rules, or can they be considered case-by-case?
While TPN contraindications typically serve as guidelines, there are instances where healthcare providers must assess the unique needs of the individual patient and make well-informed judgments.
Is TPN Contraindicated in Pregnancy?

TPN is not typically contraindicated in pregnancy, but it is generally avoided unless absolutely necessary. This is due to the fact that pregnant women usually have a working digestive system, and it is often safer for both the mother and the infant to obtain nutrients by oral intake or, if necessary, tube feeding. TPN may be used in extreme cases when the digestive system is impaired, but its use should be approached with caution given the accompanying potential hazards.
Doctors carefully weigh the benefits and risks to make the best decision for the health of the pregnant woman and her baby.
Conclusion
Healthcare professionals must possess a comprehensive understanding of TPN contraindications in order to make well-informed decisions regarding patient nutrition. TPN is a highly effective treatment, however, it does have some limitations. Recognizing when TPN is appropriate and when it should be avoided is crucial for providing the best care possible to patients.
REFERENCES:
- Hamdan, M. (2023). Total parenteral nutrition. StatPearls – NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK559036/
- Boullata JI, Gilbert K, Sacks G, Labossiere RJ, Crill C, Goday P, Kumpf VJ, Mattox TW, Plogsted S, Holcombe B. (2014). American Society for Parenteral and Enteral Nutrition. A.S.P.E.N. clinical guidelines: parenteral nutrition ordering, order review, compounding, labeling, and dispensing. JPEN J Parenter Enteral Nutr. 38(3):334-77.
- Total parenteral nutrition in pregnancy: case review and guidelines for calculating requirements. (1997). PubMed. https://doi.org/10.1002/(SICI)1520-6661(199707/08)6:4
- Maudar KK. (1995). Total Parenteral Nutrition. Med J Armed Forces India. 51(2):122-126. https://doi.org/10.1016/S0377-1237(17)30942-5