Total Parenteral Nutrition (TPN), an established medical intervention introduced in the 1960s, has played a pivotal role in saving lives. TPN infusion therapy serves the purpose of directly supplying vital nutrients into the bloodstream of patients who suffer from profound gastrointestinal disorders or have undergone extensive bowel surgery, thus rendering their digestive system incapable of effectively absorbing or processing food. While TPN plays a critical role in providing essential nourishment to facilitate healing and promote overall well-being, it is not without potential risks and complications. Among these, the most notable concern is the possibility of liver damage or, in severe cases, liver failure, particularly among individuals receiving long-term TPN treatment.
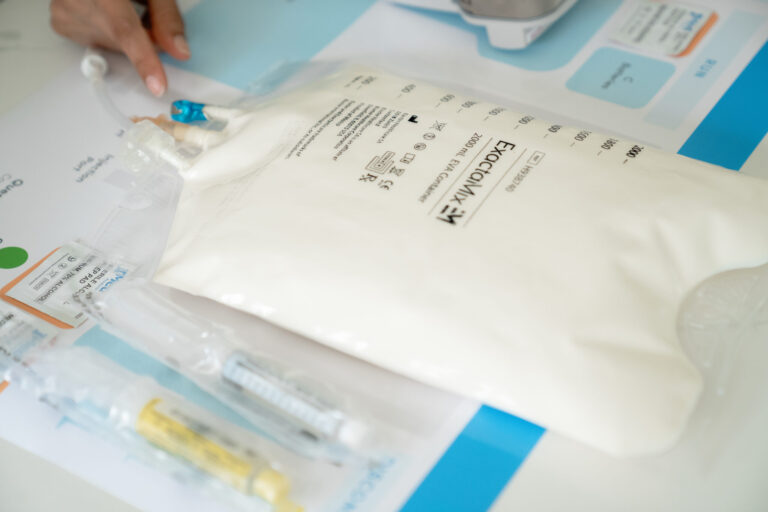
Always in Stock
Full inventory of IV fluids, ready for youAs you may already be aware, the liver holds paramount importance as an organ entrusted with the crucial task of nutrient processing. However, when the body’s customary digestive processes are circumvented, it can have detrimental consequences on the liver.
In this article, we will investigate the association between TPN and liver damage, examine probable causes of liver damage, and offer measures to reduce the potential harm to this vital organ. Getting thorough knowledge will help ensure the safest and most productive management of long-term TPN treatment for yourself or your loved ones.
How Does TPN Cause Liver Damage?
Typically, the liver plays a vital role in the metabolism of nutrients, including glucose, amino acids, and fat. By administering these nutrients directly into the bloodstream via TPN, the liver is circumvented, resulting in an augmented metabolic burden on this vital organ. This heightened metabolic load has the potential to induce liver damage, particularly when the liver is already compromised.
Individuals who undergo prolonged total parenteral nutrition (TPN) treatment face an increased risk of developing specific liver complications known as parenteral nutrition-associated liver disease (PNALD). PNALD encompasses a range of liver issues, including steatosis (fatty liver), cholestasis (disrupted bile flow), disruptions in glucose and lipid metabolism, cirrhosis (liver scarring), portal hypertension (elevated blood pressure in the liver), and, ultimately, liver failure.
The incidence of PNALD is significantly higher in infants compared to adults, with rates ranging from 40% to 60% in infants and 15% to 40% in adults. Moreover, the occurrence of PNALD rises as the duration of TPN increases.
Factors That Contribute to Liver Damage
Patients with long-term TPN use may experience liver damage or PNALD due to several factors associated with this therapy. Some of the major risk factors for liver injury in individuals taking long-term TPN include:
Composition of TPN Solution
The composition of the TPN solution plays a crucial role. High glucose, amino acids, and fat levels can overwhelm the liver’s capacity to metabolize these nutrients properly, leading to liver dysfunction over time. One prospective study reported TPN-associated liver disease in adult patients who received excessive lipids administered at >1 g/kg.
Cholestasis- The Most Common Form of Liver Damage
Cholestasis is a type of PNALD that occurs when the flow of bile from the liver is disrupted, leading to a buildup of bile in the liver. This buildup can cause inflammation and damage to liver cells, leading to liver dysfunction.
Although adults receiving TPN therapy can also experience cholestasis, it is most common in preterm newborns. In fact, cholestasis is the most common symptom of liver failure and is anticipated to affect over 70% of adult patients on long-term TPN.
Signs of cholestasis can manifest as jaundice (yellowing of the skin and eyes), darkened urine, and pale-colored stool. These symptoms indicate impaired liver function and the accumulation of bile in the liver.
Infections
Patients on long-term TPN are at an increased risk of developing infections, including bloodstream infections (sepsis). According to a study, there was a 3.2-fold higher risk of developing PNALD following an episode of sepsis. These infections can directly affect the liver and contribute to liver damage.
Nutrients Toxicity Due to Calorie Overload
The composition of the TPN solution can potentially be harmful as it may lead to calorie overload and contain components that could be toxic. Excessive feeding or overfeeding, regardless of how nutrients are given, can lead to the development of hepatic steatosis (fatty liver) and hepatitis (inflammation of the liver).
High levels and certain kinds of lipids (fats), for example, can lead to the development of hepatic steatosis. When TPN contains an excessive quantity of lipids, the liver may struggle to adequately metabolize and digest them. This can cause fat to accumulate within liver cells, resulting in hepatic steatosis and liver damage.
Hepatic steatosis during TPN may be more likely to occur due to factors such as prolonged use of TPN, elevated glucose levels in the TPN solution, insulin resistance, and the presence of underlying conditions like obesity or diabetes.
Nutrient Deficiency
Despite receiving TPN, patients may still experience deficiencies in certain nutrients. These deficiencies can further impact liver health and contribute to liver damage. These inadequacies can have an even greater impact on liver health and contribute to liver disease. Patients who take long-term TPN, for example, may have lower choline levels in their blood, which is associated with aberrant liver enzymes. As a result, choline depletion is critical in the development of TPN-associated liver illness, and it is claimed that choline is a vital component required by people receiving long-term home TPN.
Moreover, it is also important to note that not everyone on long-term TPN treatment will necessarily experience liver damage or failure. While liver complications are a known risk, the likelihood and severity can vary depending on individual factors and proper management of TPN therapy.
Speak to a Specialist
About Copay AssistanceHow to Prevent Liver Damage?
One of the most effective strategies to prevent liver damage caused by TPN is to provide nutrients in a balanced manner that mimics the body’s natural processes. Because the liver processes glucose in a controlled and regulated manner, regulating the amount of glucose administered via TPN is critical to avoid overloading the liver.
The kind and quantity of fat administered via TPN is a further crucial factor. Although fat is a necessary nutrient, an excessive amount of it can harm the liver. Therefore, it is essential to give the patient the proper ratio of omega-3 and omega-6 fatty acids and to frequently check their lipid levels.
Similarly, the proper amino acid balance via TPN is essential to avoid overloading the liver with protein. Furthermore, certain amino acids, such as glutamine, have been proven to reduce the risk of liver damage from TPN.
Hence, close monitoring of liver function, regular assessments, and adjustments to the TPN formulation can help minimize the risk and manage potential liver complications effectively.
Conclusion
In essence, TPN stands as a medical intervention that delivers vital nutrients directly into the bloodstream via an intravenous catheter. Nonetheless, the prolonged utilization of TPN carries the potential for liver damage or failure. Through a proactive approach that acknowledges and tackles these risks, it is feasible to reduce the likelihood of liver problems. Vigilant monitoring of liver function and maintaining a strong partnership with healthcare experts are crucial in detecting any issues early on and ensuring optimal management.
REFERENCES:
- Jain, A., & Teckman, J. (2014). Newly Identified Mechanisms of Total Parenteral Nutrition Related Liver Injury. Advances in Hepatology (Online), 2014, 1–7. https://doi.org/10.1155/2014/621380
- Żalikowska-Gardocka, M., & Przybyłkowski, A. (2020). Review of parenteral nutrition-associated liver disease. Clinical & Experimental Hepatology, 6(2), 65–73. https://doi.org/10.5114/ceh.2019.95528
- Chan, S., McCowen, K. C., Bistrian, B. R., Thibault, A., Keane-Ellison, M., Forse, R. A., … & Burke, P. (1999). Incidence, prognosis, and etiology of end-stage liver disease in patients receiving home total parenteral nutrition. Surgery, 126(1), 28-34. https://doi.org/10.1067/msy.1999.98925
- Bellamy, C., & Burt, A. D. (2018). The Liver in Systemic Disease. In Elsevier eBooks (pp. 966–1018). https://doi.org/10.1016/b978-0-7020-6697-9.00015-7
- Raman, M., & Allard, J. P. (2007). Parenteral nutrition related hepato-biliary disease in adults. Applied Physiology, Nutrition, and Metabolism, 32(4), 646–654. https://doi.org/10.1139/h07-056