Individuals with chronic immune conditions typically require Ig therapy almost regularly for a long period to maintain their health and improve their quality of life.
Home Infusion – We Come To You
Initially, Ig therapy was only given in a hospital setting as a safety precaution to manage adverse effects if they occur. However, with recent advancements in medical technology, patients can now easily receive Ig therapy in the comfort of their homes without missing any scheduled infusions.
In this article, we’ll review the long-term benefits of receiving Ig therapy at home and how it supports both ongoing health and an improved quality of life among Ig patients.
Understanding Ig Therapy
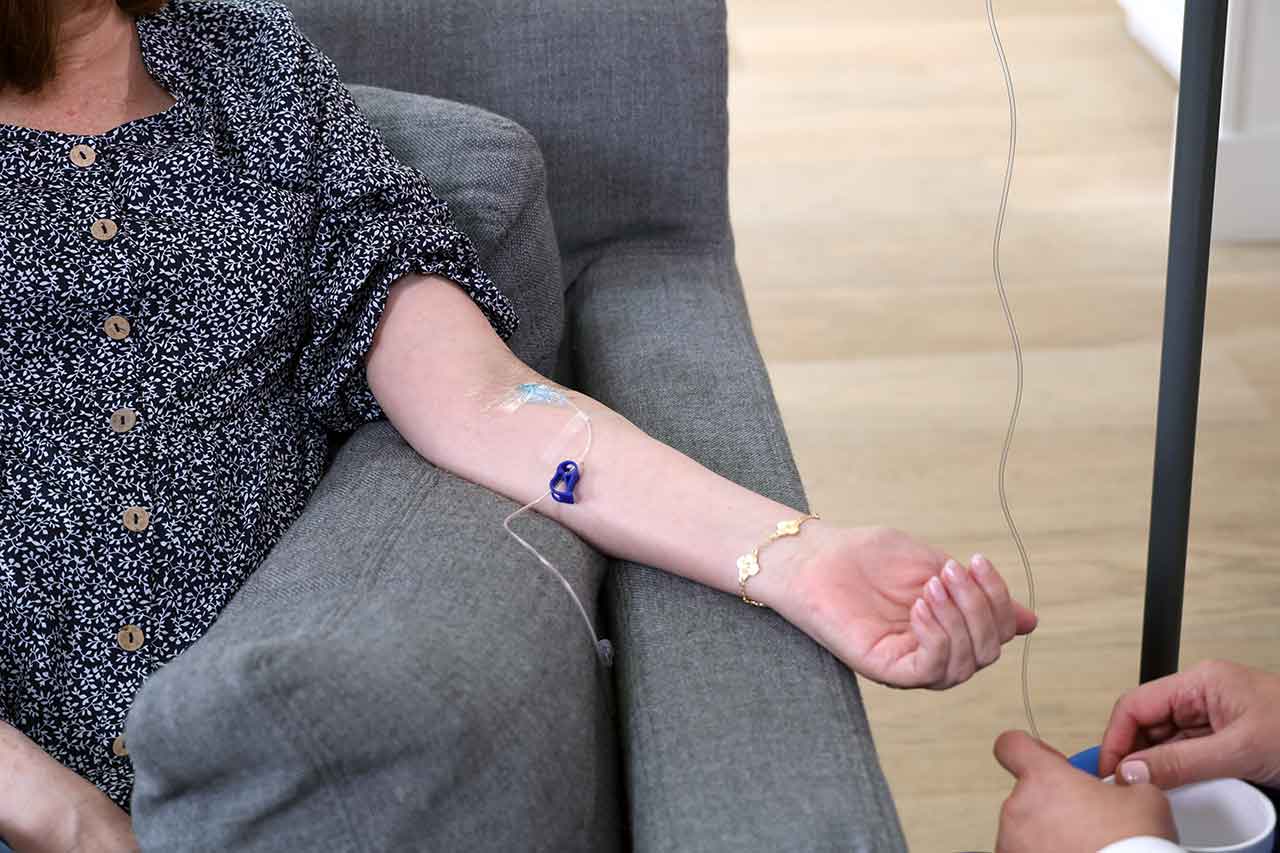
Ig therapy provides immunoglobulins (antibodies), which are obtained from healthy donors and either administered intravenously (IVIG) or subcutaneously (SCIG). These antibodies are used to strengthen the immune systems of people who either lack essential antibodies or have dysfunctional immune systems (i.e., immune systems that work abnormally).
For these patients, Ig therapy becomes a life-long treatment that must be continued to maintain ongoing health and improve quality of life by preventing infections and managing disease-associated symptoms effectively.
Currently, Ig therapy can be delivered at different care sites, including physicians’ offices, outpatient departments of hospitals, and if well-tolerated, at patients’ homes. Most patients with life-long immune conditions preferred receiving Ig infusions in the comfort of their homes due to the potential long-term benefits, ranging from improved quality of life and physical well-being to reduced financial burden.
Long-Term Benefits of Ig Therapy at Home
Some of the significant long-term benefits of receiving Ig therapy at home are as follows:
1. Enhanced Comfort and Convenience
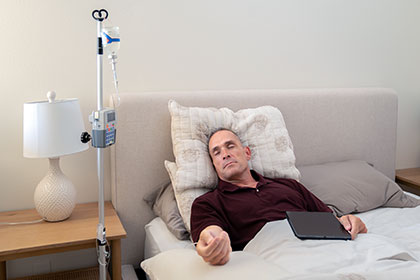
Home-based Ig therapy provides enhanced comfort and convenience compared to traditional hospital-based infusions. Patients can easily incorporate the Ig treatment into their daily routine without worrying about spending hours traveling to and from hospitals regularly, which is particularly burdensome for individuals with mobility issues or those living far from healthcare centers.
Moreover, the continuous support and love from family at home also help patients to relax in their own space and alleviate anxiety, which often impacts Ig patients in clinical settings. The home care approach of Ig therapy not only promotes a positive mindset but also enhances patient adherence to their treatment, contributing to their overall long-term health.
2. Reduced Financial Burden
Home Ig therapy reduces the financial burden on patients and their caregivers because receiving Ig infusions at home is less expensive than receiving it in a hospital setting or infusion center. For instance, according to one observational study, a home Ig infusion cost was $1,452, which is 31% cheaper than an outpatient infusion. A single patient undergoing 13 to 18 home infusions a year can save an estimated $18,876 to $26,136 annually.
The cost of Ig infusion at home may vary and may depend on the type of delivery method (IVIG or SCIG). For example, the cost-effectiveness of moving IVIG to the home environment and even switching patients from IVIG to SCIG has been demonstrated in numerous studies.
If you have a primary immunodeficiency (PI) disorder, you can enroll in a Medicare insurance program. Under the Consolidated Appropriations Act of 2023, Medicare now permanently covers home IVIG therapy with full support, including professional care and all the supplies you need.
Speak to a Specialist
About Copay Assistance3. Decreased Risk of Infections

Another long-term benefit of receiving Ig therapy at home is less exposure to potentially harmful pathogens and lower rates of hospital-acquired infections. Unlike the hospital or clinical settings, which are breeding grounds for harmful infections, patients with weak immune systems (e.g., primary or secondary immunodeficiency disorders) can receive their scheduled Ig doses at home in a safe and clean environment.
A study reported that patients who received home-based infusion had significantly lower rates of bronchitis and pneumonia compared to the rates at an outpatient hospital. However, some patients may still experience infection if proper aseptic protocol is not followed.
4. Improved Quality of Life
Beyond the comfort and convenience, patients who received Ig therapy at home for a long period reported significantly improved quality of life due to greater control over day-to-day activities.
For example, with home infusions, patients no longer need to visit the hospital for Ig administration and can easily receive treatment at home at their scheduled time. This allows patients to engage in leisure and travel activities, which consequently improves their mental health and reduces stress.
Furthermore, a study reported that patients who received consistent Ig therapy at home without missing any scheduled doses experienced better health outcomes and improved quality of life, including significantly improved symptoms, fewer infections, and fewer hospitalizations.
5. Personalized Care
Home Ig therapy provides personalized care to support the patient’s ongoing health. In a personalized care approach, the treatment plan is tailored according to the needs of the patient throughout their life. Highly trained nurses regularly monitor the patient’s condition and infusion process and provide one-on-one care to address any concerns.
Moreover, nurses educate patients or caregivers about safely infusing Ig doses and monitoring their conditions. This collaborative approach promotes better health outcomes and helps patients feel more in control of their condition.
Eligibility of Receiving Ig Therapy at Home
Not every patient is eligible or suitable for home Ig therapy. For instance, home Ig therapy is mainly recommended to patients with primary or secondary immunodeficiency or life-long neurological autoimmune disorders who require this therapy for the long term. Home Ig therapy is recommended to limit frequent hospital visits and save time, travel expenses, and healthcare costs.
The decision to transition Ig treatment from hospital to home care is made collaboratively by healthcare providers and the patient based on the patient’s medical condition, stability, and ability to manage home therapy safely.
Ask About IVIG Home Infusion
Conclusion
In summary, home Ig infusions offer various long-term benefits, such as providing comfort and personalized care, easing financial burden, and reducing hospital stays and risk of infections, making it an optimal choice for many Ig patients. These long-term benefits not only enhance patient care and quality of life but also promote a feeling of independence among Ig patients.