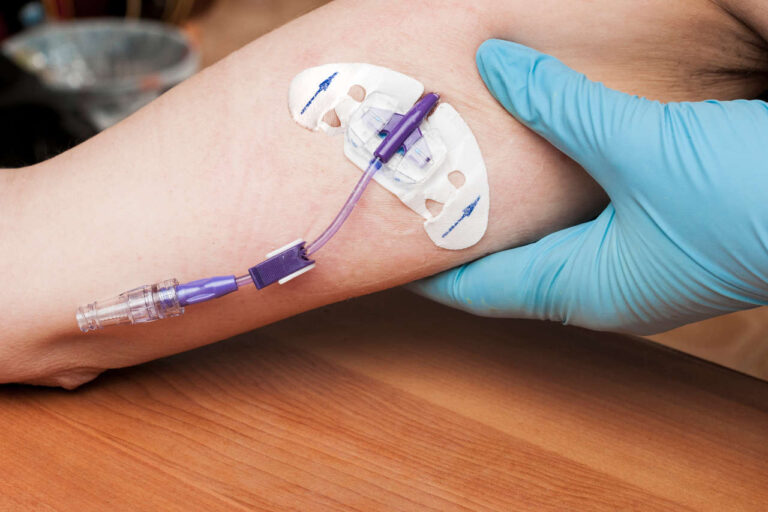
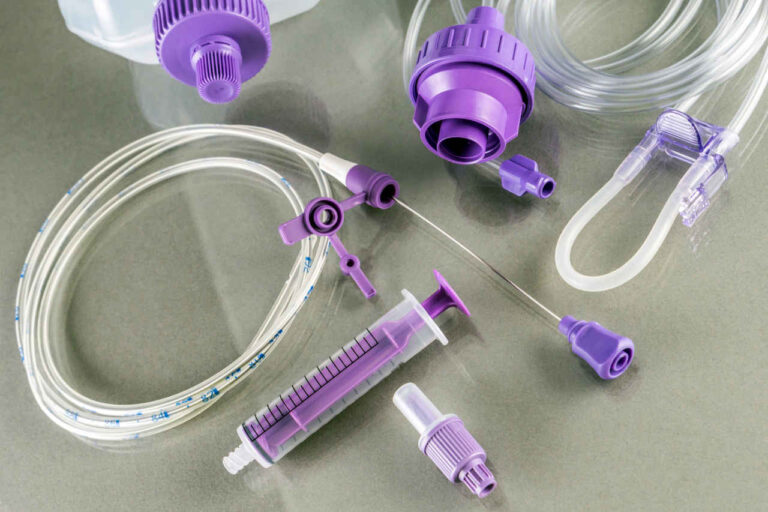
Total parenteral nutrition (TPN) can be lifesaving for people who cannot or should not use their digestive systems for feeding. Unfortunately, long-term TPN is known to cause a potentially serious complication called TPN-induced cholestasis.
Speak to a Specialist
About Copay AssistanceOther names for the condition are:
- Nutrition–associated cholestasis (PNAC)
- Intestinal failure–associated liver disease (IFALD)
- Parenteral nutrition–associated liver disease (PNALD)
In this article, you will find evidence-based answers to the most common questions about this condition.
1. What is TPN-Induced Cholestasis?
TPN-induced cholestasis is a well-established complication of long-term TPN use. It usually occurs within 1 to 4 weeks after starting TPN.
Cholestasis is when bile flow slows down either because your liver makes less bile or the tubes that carry bile (bile ducts) become obstructed.
TPN-induced cholestasis is a medical condition characterized by elevated levels of bilirubin (yellowish pigment) and liver enzymes. High blood levels of bilirubin can lead to jaundice, which causes yellow skin and eyes.
A 2016 review in Clinics in Liver Disease reports that jaundice is rare in adults but occurs in up to 50% of children during TPN therapy. [1]
2. How Common is It?
Children are more likely than adults to develop this condition. According to a 2022 study in the journal Cureus, 18% to 67% of infants who receive TPN for over 14 days are at risk of getting liver injury and cholestasis. [2]
Likewise, in acute care settings, over 30% of adults on TPN therapy develop cholestasis. [3]
3. How Does TPN Cause Cholestasis?
Cholestasis of TPN can occur due to a multitude of factors. [1,4,5,6] These include:
Patient Factors
Unlike adults, neonates have immature enterohepatic circulation, resulting in impaired bile release and uptake. This phenomenon might explain why this condition is more common in premature babies.
Role of Nutrients
Excessive calories: Patients on TPN often receive excessive calories, which requires the pancreas to make more insulin than usual. On top of this, many patients are traumatized and typically have insulin resistance.
The cumulative effect is that these individuals have high levels of insulin, which cause fats (lipids) to accumulate in the liver. Consequently, an inflammatory reaction starts in the liver cells, possibly leading to their scarring (cirrhosis).
Excessive lipid infusion: The exact effect of excessive lipid infusion is unclear. However, cholestasis is thought to result due to accumulation of excess lipids in liver cells.
Amino acids: Excess glycine and deficiency of sulfur-containing amino acids in the TPN formulation may lead to the formation of insoluble bile acid products, which may promote cholestasis.
Bacterial Overgrowth and Endotoxins
Bacterial overgrowth and endotoxins in the intestines may promote cholestasis in some patients.
Other Potential Factors
Researchers are investigating the potential role of the gut microbiome (collection of microbes in the gut) in cholestasis associated with TPN.
Ask About TPN Home Infusion
4. What Are the Risk Factors?
In preterm babies, the two strongest predictors of cholestasis are low birth weight and duration of TPN therapy. [7]
According to a team of American investigators, the risk of cholestasis is highest among babies with a birth weight of less than 500 g. In addition, they report that the longer the duration of TPN therapy, the higher the incidence. [8]
In adults, the most common risk factors [3] are:
- Severe malnutrition
- Infection
- High carbohydrate and fat intake
5. What Are the Complications?
Excess lipid deposition in liver cells and inflammatory reactions can lead to complications, such as fibrosis and cirrhosis. They are most likely to occur if cholestasis persists, especially among children on TPN.
Fibrosis
Fibrosis—the first stage of liver scarring—occurs when scar tissues replace healthy liver cells. As a result, the liver cannot function normally.
Mild to moderate cases often have no symptoms, while some people may complain of:
- Appetite loss
- Swollen legs or stomach
- Jaundice
- Nausea
- Unexplained weight loss
- Weakness
Fibrosis may sometimes reverse with appropriate treatment.
Cirrhosis
Cirrhosis is a severe form of fibrosis that is usually irreversible. Early stages often produce no symptoms. However, as the disease progresses, you may experience:
- Appetite loss
- Nausea
- Upper abdominal pain on the right side
- Visible spider-like vessels
Diet and lifestyle changes, along with specific medications, may help delay progression. Nonetheless, surgery may be required if you do not respond to treatment or develop liver failure.
Chronic liver failure may occur in 3% to 15% of affected children. [8]
AmeriPharma™ Specialty Care
otal Parenteral Nutrition | Leader In TPN Assistance6. How Is TPN-Induced Cholestasis Diagnosed?
Your doctor will start with a medical history review and physical examination. Also, they will probably ask if you have taken any herbal supplements recently. Note that these supplements, which are not regulated by the U.S. FDA, may contain chemicals toxic to your liver.
Then, they will order an ultrasound of the liver and biliary system to check if you have any obstructions in the bile ducts. Sometimes, you may need another advanced imaging test called magnetic resonance cholangiopancreatography (MRCP).
Your doctor will test your blood sample to determine liver enzymes, bilirubin, and the presence of the hepatitis virus. Other tests may include:
- CT scan of the abdomen
- Barium studies
If the diagnosis is still unclear, you may have to go for a liver biopsy. A liver biopsy examines liver cells under a microscope to look for signs of liver damage or disease.
7. What Are the Treatments for TPN-Induced Cholestasis?
If diagnostic tests show TPN as the sole cause of cholestasis, your doctor will review total calorie intake and adjust the mix to prevent high carbohydrate and fat infusion. They may also add trace elements like zinc, selenium, and chromium to the mix.
If you have bacterial overgrowth, you may be given antibiotics, including metronidazole (brand name: Flagyl).
Other medicines that may help treat or manage cholestasis include carnitine (brand name: Carnitor) and ursodeoxycholate (most commonly known as ursodiol, brand name: Actigall).
A liver transplant remains the last resort for treatment.
REFERENCES:
- Beath, Sue V, and Deirdre A Kelly. “Total Parenteral Nutrition-Induced Cholestasis: Prevention and Management.” Clinics in liver disease vol. 20,1 (2016): 159-76. doi:10.1016/j.cld.2015.08.009
- Al-Alaiyan, Saleh et al. “Ursodeoxycholic Acid and SMOFlipid for Treating Parenteral Nutrition Associated Cholestasis in Infants.” Cureus vol. 14,2 e22060. 9 Feb. 2022, doi:10.7759/cureus.22060
- Lakananurak, Narisorn, and Kakanan Tienchai. “Incidence and risk factors of parenteral nutrition-associated liver disease in hospitalized adults: A prospective cohort study.” Clinical nutrition ESPEN vol. 34 (2019): 81-86. doi:10.1016/j.clnesp.2019.08.009
- Guglielmi, Francesco William et al. “Cholestasis induced by total parenteral nutrition.” Clinics in liver disease vol. 12,1 (2008): 97-110, viii. doi:10.1016/j.cld.2007.11.004
- Tomar, B.S. Hepatobiliary abnormalities and parenteral nutrition. Indian J Pediatr 67, 695–701 (2000). https://doi.org/10.1007/BF02762189
- Jeejeebhoy, Khursheed N. “Management of PN-induced cholestasis.” Pract Gastroenterol 24 (2005): 62-68.
- Alkharfy, Turki M et al. “Total parenteral nutrition-associated cholestasis and risk factors in preterm infants.” Saudi journal of gastroenterology : official journal of the Saudi Gastroenterology Association vol. 20,5 (2014): 293-6. doi:10.4103/1319-3767.141688
- Christensen, R D et al. “Identifying patients, on the first day of life, at high-risk of developing parenteral nutrition-associated liver disease.” Journal of perinatology : official journal of the California Perinatal Association vol. 27,5 (2007): 284-90. doi:10.1038/sj.jp.721168