Though not routinely used after bariatric surgery, TPN (total parenteral nutrition) may help certain patients with surgery-related complications and severe malnutrition.
Get Copay Assistance Now
What Is TPN?
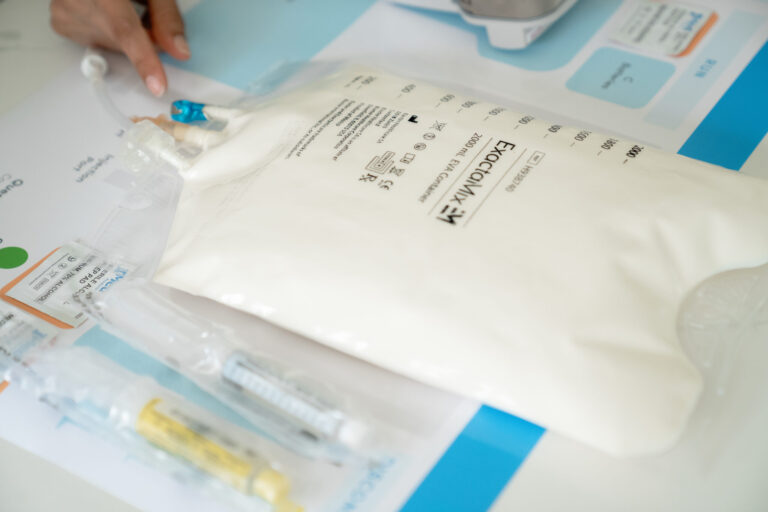
Total parenteral nutrition (TPN) is a feeding method that bypasses the digestive tract. It involves administering a special formula directly into your bloodstream through a vein. The formula contains fats, sugar, protein, salts, vitamins, minerals, and water. Thus, TPN provides most nutrients your body needs to function.
What Is Bariatric Surgery?
Bariatric surgery (also called weight loss surgery or metabolic surgery) is a type of obesity treatment. It involves surgical procedures that make changes in the digestive tract. These changes can help you lose weight by:
- Limiting the number of calories you can take in and absorb
- Reducing hunger signals
Bariatric surgery may be done when other weight loss treatments have failed or when you have serious obesity-related health issues. According to the American Society for Bariatric and Metabolic Surgery, over 270,000 surgeries were performed in 2023 [1].
Bariatric Surgery Complications
While bariatric surgery can help you lose weight, it’s no quick fix. Besides, it comes with potential side effects, such as:
- Malabsorption (impaired absorption of nutrients by the small intestine)
- Malnutrition (deficiency of nutrients)
- Gallstones (hardened deposits in the gallbladder or bile ducts)
- Bile reflux (upward flow of bile from the small intestine into the stomach)
- Bleeding
- Infection
- Blood clots
- Small bowel obstruction (blockage in the small intestine)
- Anastomotic leaks (leaks from the surgically reconnected region of the intestine)
When May TPN Be Used After Bariatric Surgery?
TPN isn’t generally used after bariatric surgery. That said, TPN may be an option when patients have severe surgery-related complications or malnutrition following surgery.
TPN for Post-Surgery Malnutrition
Individuals who have had bariatric surgery may have malabsorption severe enough to cause malnutrition. They may be deficient in nutrients, including [2]:
- Vitamins like A, D, B12, thiamine, and folic acid
- Minerals like zinc, copper, and iron
- Protein (often causing hair loss)
- Fat
Speak to a Specialist
About Copay AssistanceMoreover, some people who have undergone bariatric surgery may develop something called “failure to thrive” or FTT. This is a potentially life-threatening condition characterized by extensive weight loss, frequent vomiting, and malnutrition.
Extremely low albumin (a protein) levels in the blood are another complication associated with certain types of weight-loss surgery [3].
TPN can help correct deficiencies and increase weight and serum albumin levels. In a 2016 study, researchers analyzed the data of 54 patients with a history of bariatric surgery who were given home parenteral nutrition (HPN).
By the end of the HPN treatment, they found that participants who received HPN had significantly higher weight gain and serum albumin levels [4].
Considering these benefits, parenteral nutrition may be used to:
- Correct nutritional deficiencies
- Increase serum albumin levels
- Prepare patients for revisional bariatric surgery (surgical procedures after weight loss surgery to reduce side effects)
TPN for Surgery-Related Complications
An anastomotic leak is an early complication associated with bariatric surgery. It can cause bowel contents to leak into the abdominal cavity, potentially leading to infection. Leakage occurs from the surgically reconnected region of the intestine.
TPN is often the most preferred feeding method in such cases because it allows anastomotic leaks to heal by providing rest to the gut. Some healthcare providers may find TPN easier to administer than other feeding methods [5].
TPN for Chronic Intestinal Failure After Bariatric Surgery
Individuals who have had weight loss surgery may be at a higher risk of developing chronic intestinal failure, which requires long-term parenteral support.
Chronic intestinal failure is a long-term condition. Individuals with this condition cannot absorb the bare minimum of nutrients, water, and salts necessary to maintain health or growth. So, they require TPN for extended periods, until other remedial actions are taken.
Note: Chronic intestinal failure is different from intestinal insufficiency, which doesn’t require parenteral support for health or growth.
In these patients, TPN is well tolerated and effective regardless of the type of weight-loss surgery [6].
What Are the Side Effects of TPN After Bariatric Surgery?

Side effects experienced while receiving TPN after bariatric surgery are generally similar to those associated with TPN in other settings. These may include:
- Nausea or vomiting
- Increased urination
- Swelling of the hands, feet, or legs
- Stomach pain
- Tingling in the hands or feet
- Fever or chills
- Mouth sores
- Skin changes
- Rapid weight loss or gain
- Muscle weakness
- Catheter obstruction
- Liver disease
- Osteoporosis (brittle bones)
Get Financial Assistance
Duration of TPN After Bariatric Surgery
Due to limited data, it’s not possible to pinpoint the exact duration of TPN therapy after bariatric surgery. Moreover, several factors can affect the duration, the most important being the condition for which TPN is used.
For example, TPN treatment may last several months in a patient with intestinal failure after bariatric surgery. On the other hand, patients with infection due to anastomotic leaks may need TPN for about a month or two.
TPN After Bariatric Surgery: Frequently Asked Questions
What are the benefits of using TPN after bariatric surgery?
TPN after bariatric surgery can help correct nutritional deficiencies, improve albumin levels, and act as a “bridge” for revisional surgery.
What are the dietary guidelines after bariatric surgery?
The general guidelines recommend [7]:
Do’s:
- Eat a balanced diet (low in calories, fats, and sugars) with small portions.
- Record your food portions and calorie and protein intake daily.
- Eat slowly and chew properly.
Don’ts:
- Eat foods that are hard to chew. These include rice, bread, raw vegetables, fresh fruits, and meat.
- Use straws, drink fizzy drinks, or chew ice. They can cause discomfort.
- Consume sugar, sugar-containing foods and beverages, concentrated sweets, and fruit juices.
During the first 60 days after surgery, maintain your daily calorie intake between 300 and 600 calories. Don’t consume more than 1,000 calories a day.
What is the most common cause of death after gastric bypass surgery?
Pneumonia and other respiratory conditions are most commonly associated with death after bypass surgery. Smoking, heart disease, and high blood pressure can increase the risk.
REFERENCES:
- “Estimate of Bariatric Surgery Numbers, 2011-2023 – American Society for Metabolic and Bariatric Surgery.” American Society for Metabolic and Bariatric Surgery, 14 Apr. 2025, asmbs.org/resources/estimate-of-bariatric-surgery-numbers.
- Ganipisetti VM, Naha S. Bariatric Surgery Malnutrition Complications. [Updated 2023 May 19]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK592383/#
- Santos Reis, Catarina et al. “Severe Hypoalbuminaemia after Roux-En-Y Gastric Bypass: A Diagnosis of Exclusion.” European journal of case reports in internal medicine vol. 12,9 005741. 25 Aug. 2025, doi:10.12890/2025_005741
- Mundi, Manpreet S., et al. “Use of Home Parenteral Nutrition in Post–Bariatric Surgery–Related Malnutrition.” Journal of Parenteral and Enteral Nutrition, vol. 41, no. 7, May 2016, pp. 1119–24, doi:10.1177/0148607116649222.
- Segaran, Ella. “Provision of Nutritional Support to Those Experiencing Complications Following Bariatric Surgery.” Proceedings of the Nutrition Society, vol. 69, no. 4, Aug. 2010, pp. 536–42, doi:10.1017/s0029665110001965.
- Daoud, Dane Christina, et al. “Long‐term Home Parenteral Nutrition in Chronic Intestinal Failure Following Metabolic and Bariatric Surgery and Its Clinical Outcomes: A Descriptive Cohort Study.” Journal of Parenteral and Enteral Nutrition, vol. 49, no. 6, May 2025, pp. 773–82, doi:10.1002/jpen.2772.
- UCSF Health. “Dietary Guidelines After Bariatric Surgery.” ucsfhealth.org, 21 May 2024, www.ucsfhealth.org/education/dietary-guidelines-after-bariatric-surgery.