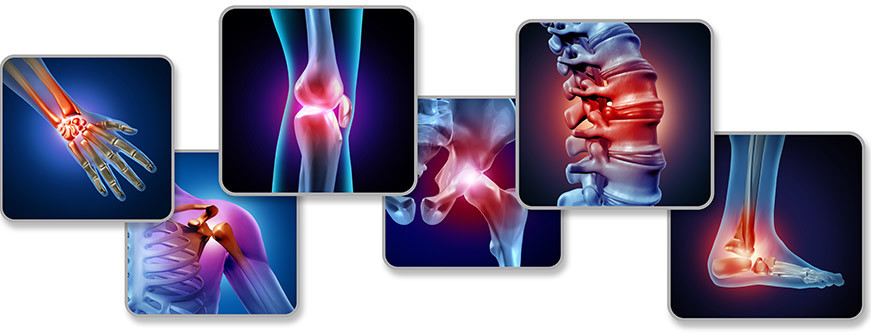
Incessant inflammation can go from discomforting to downright painful very quickly. When it occurs at the joints, it could be a sign of rheumatoid arthritis. This disease can cause severe pain from simple actions like bending the knee or attempting to hold a pen.
What Is Rheumatoid Arthritis?
A healthy, functioning immune system attacks harmful bacteria and viruses to protect the body from illness. However, in autoimmune diseases, the immune system, which is intended to protect you, begins to attack healthy parts of the body.
Rheumatoid arthritis is a chronic autoimmune disease where the immune system erroneously attacks the joints, causing inflammation to the tissue lining that protects the joints and enables movement. If untreated, the inflammation can cause pain, swelling, stiffness, and, in severe cases, joint deformity and other life-threatening complications.
Get IVIG Copay Assistance
IVIG Financial AssistanceCauses and Risk Factors
Doctors have not yet been able to identify what triggers the immune system to malfunction and attack the body. However, they have been able to locate a few risk factors associated with rheumatoid arthritis. These include:
- Your sex. According to WebMD, the disease is two to three times more common in women than in men.
- Your age. Rheumatoid arthritis commonly develops in middle age, although it has been found to affect people of all ages.
- Family history. If someone in your family has rheumatoid arthritis, you have an increased risk for the disease.
- Whether you smoke. Smoking cigarettes can increase the likeliness of developing the disease, especially if you have a family history. It has also been shown that smoking can impact the severity of the disease as well.
- How much you drink. Heavy alcohol intake is suspected to be a trigger for rheumatoid arthritis. It is important to note, however, that some studies suggest moderate alcohol intake may have a protective effect. Therefore, if you do drink, please do so in moderation.
- Environmental exposure. Those exposed to asbestos or silica have a higher risk for rheumatoid arthritis. Recent studies have shown that exposure to air pollution and toxic chemicals can also be contributing factors.
- Your weight. Being overweight can increase your risk of disease.
Those with multiple risk factors are at an even higher risk of developing the disease.
Rheumatoid Arthritis Signs, Symptoms, and Complications

People who develop rheumatoid arthritis will likely experience joint pain and swelling, stiffness typically following long periods of inactivity, fatigue, fever, and loss of appetite. If these symptoms persist for 6 weeks or longer, it could be rheumatoid arthritis, and you should schedule an appointment with your doctor right away.
If untreated, the disease can worsen significantly over time. As the joint lining diminishes, bone erosion can occur, leading to osteoporosis and joint deformity. Furthermore, if the malfunctioning immune system is not controlled, it can affect other important areas of the body including the eyes, skin, mouth, lungs, and more.
Get IVIG Copay Assistance
Your IVIG Treatment Info | Get IVIG Prior AuthorizationGetting Diagnosed
During your exam, your doctor will look for joint swelling, redness, and warmth in the affected areas. They will also check your reflexes and muscle strength. You will need blood tests to look for signs of inflammation, low red blood cell count, and certain antibody levels.
Treatment Options
Once diagnosed, a treatment plan will be prescribed by your doctor to help manage the symptoms and prevent complications. Common medications include anti-inflammatory pain killers, topical pain relievers, and corticosteroids. You may also be prescribed disease-modifying antirheumatic drugs (DMARDs), which work to suppress the immune system’s attack of the joint lining. The preferred initial treatment for rheumatoid arthritis is a DMARD called methotrexate. This drug is often prescribed immediately after diagnosis because early use leads to better long-term results.
Biologic response modifiers (a faster-acting type of DMARD) are often used for patients with a more severe form of rheumatoid arthritis and for patients whose symptoms are not controlled with DMARDs. Biologics are administered as an injection or infusion in a doctor’s office. In some instances, joint replacement surgery may be recommended to help improve mobility.
It is important to note that RA treatment plans are highly individualized, and the choice of therapy depends on a number of factors, such as disease severity, comorbidities, and other factors.
Lifestyle Changes
In addition to receiving the treatments discussed above, certain lifestyle changes can improve rheumatoid arthritis symptoms and overall health. Some of the lifestyle changes you can make include:
- Diet: While there is no special diet to cure rheumatoid arthritis, eating a healthy, well-balanced diet can have many benefits. Because RA is an inflammatory disease, following an anti-inflammatory diet such as the Mediterranean diet, can help immensely. Maintaining a healthy diet helps prevent excess weight gain, which is important because extra weight can strain your joints and increase inflammation.
- Exercise: Regular exercise is strongly encouraged for RA patients as it can help maintain joint health and strengthen muscles. Types of exercises that can be helpful include low-impact aerobic exercises (like walking or swimming), flexibility exercises (like yoga or stretching), and strength training.
- Physical Therapy: Working with a physical therapist can be beneficial in a couple of different ways. First, they can create tailored exercises that will help improve joint range of motion, muscle strength, and endurance. Second, they can help you manage pain by using heat or ice packs, as well as using devices such as a TENs (transcutaneous electrical nerve stimulation) machine.
Conclusion
If you suspect you may have rheumatoid arthritis, the best thing to do is see your doctor right away. The earlier the disease is diagnosed, the better you can prevent irreversible damage from occurring.