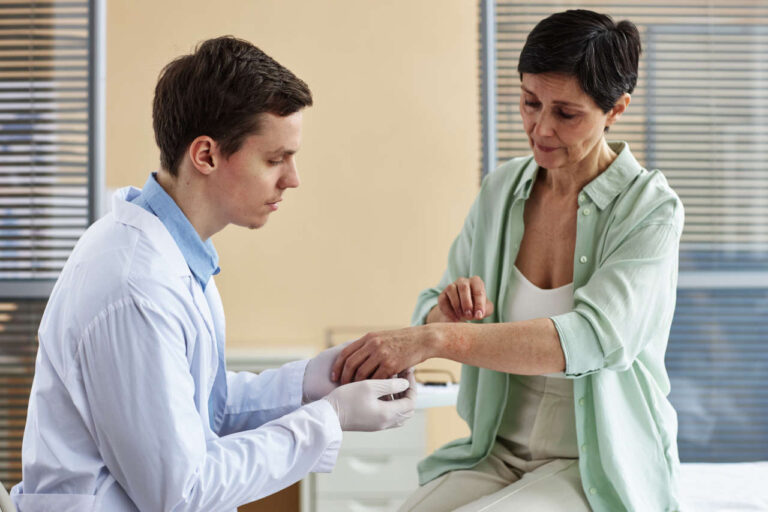
Did you know that suddenly eating food after a long period of malnourishment, extreme dieting, or starvation can be life-threatening? This is a serious condition known as refeeding syndrome.
Always in Stock
Full inventory of IV fluids, ready for youA study showed that the mortality (death) rate in people who experienced refeeding syndrome was 71%. This condition can happen to anyone at any age. Hence, it’s absolutely critical to have a proper nutritional assessment and be closely monitored by healthcare professionals after going through an extended period of fasting for any reason.
In this article, we will discuss all the details about what refeeding syndrome is and its causes, symptoms, treatment, and prevention.
What Is Refeeding Syndrome, and How Does It Occur?
Refeeding syndrome is a group of symptoms that occur when a severely nutrient-deprived or malnourished person is suddenly given carbohydrate and nutrient-rich food. Refeeding syndrome occurs because of the sudden shift of your body’s fluids and electrolytes because it has to change its mechanisms for converting nutrients into energy.
Normally, our body uses energy from the essential nutrients and ingredients in the food we eat, like carbohydrates, fibers, vitamins, and proteins. But when you suddenly stop eating food, for example, in case of starvation, malnourishment, or fasting, the body utilizes stored carbohydrates, fats, and proteins as sources of energy. Your body’s electrolyte stores are also depleted, and the amount of insulin your body secretes is lowered.
When you start eating food again, the body has to shift its mechanism from using stored macronutrients (e.g., sugars, fats, proteins) for energy to using the nutrients from the food to give your body energy. This sudden shift to carbohydrate metabolism from fat metabolism causes a group of symptoms called refeeding syndrome.
Symptoms of Refeeding Syndrome

The symptoms of refeeding syndrome can vary from person to person. But the typical symptoms include:
- Confusion
- Fatigue
- Breathing difficulty
- Seizures
- High blood sugar
- High blood pressure
- Weakness
- Acute heart failure
- Coma or death
Refeeding syndrome can also lead to low electrolyte levels, such as low levels of potassium, magnesium, and phosphate, which can cause the following symptoms:
- Excessive urination
- Paralysis
- Slowed breathing rate
- Cardiac arrest
- Blockage in the intestine (ileus)
- Nausea and vomiting
- Weakness and fatigue
- Abnormal heart rhythms
- Low levels of calcium
Since low electrolyte levels can be life-threatening in people with refeeding syndrome, usually healthcare providers will monitor blood electrolyte levels closely and replenish them as needed.
Ask About TPN Home Infusion
Risk Factors of Refeeding Syndrome
The following factors can raise the risks for refeeding syndrome when food is re-administered.
- If you have continuously consumed very little food that is rich in carbohydrates, fats, calories, proteins, and fibers for the past 10 days or more and then you suddenly start taking proper and regular meals.
- If you suffered from any chronic disease and were unable to consume proper food and maintain a healthy diet.
- If you lost more than 15% of weight in the last 3 to 6 months.
- If you have low levels of potassium, magnesium, or phosphate in your blood. This can be checked through a blood test.
Other risk factors include:
- Malnourishment
- Anorexia nervosa
- Uncontrolled diabetes
- Recent surgery
Two or more of the following factors can also increase the risks of refeeding syndrome:
- A BMI (body mass index) less than 18.5
- A history of alcohol-use disorder or using certain medications for the long-term, like diuretics, insulin, antacids, or chemotherapy drugs.
- Losing more than 15% of your body weight from the past 3-6 months.
- Consuming very little food constantly for the past 5 days or more.
Diagnosis of Refeeding Syndrome
The diagnosis of refeeding syndrome involves the combination of:
- Medical history: The healthcare provider should identify and assess the patient’s disease history, underlying medical condition, and nutritional status, including any recent period of fasting, malnourishment, or severely restricted carbohydrate or calorie intake.
- A thorough physical examination of the patient: Assess the patient’s overall health condition and check for signs of malnutrition, muscle wasting, weakness tremors, fluid retention, cardiac irregularities, or other related signs of refeeding syndrome.
- Laboratory Tests: Lab tests include complete blood count (CBC), checking electrolyte levels, liver function test, blood glucose, and renal function tests. The evaluation of blood levels of nutrients, vitamins, and minerals is also crucial for identifying refeeding syndrome.
- ECG (electrocardiogram): ECG is performed to assess cardiac functions and detect any heart abnormalities.
Treatment
If a patient is experiencing signs of refeeding syndrome and has major risk factors, like weight loss, malnourishment, fasting, or starving for extended periods, it is crucial to first monitor electrolyte levels, urine and blood analysis, body functions, and conduct an overall assessment of their health condition until full recovery.
The treatment of refeeding syndrome includes administering electrolytes and vitamins intravenously. The electrolyte infusions for potassium, magnesium, and phosphate are typically at a slow rate and the doses are calculated based on body weight. Sodium replacement should be carefully monitored, especially in patients facing heart-related complications or heart disease.
People with breathing issues might require proper ventilation and oxygen supply. The treatment of refeeding syndrome varies according to individual needs and is done according to the symptoms of the patient.
AmeriPharma® Specialty Care
Total Parenteral Nutrition | Leader In TPN AssistancePrevention
The most important tip to prevent refeeding syndrome is controlling the risk factors that can cause this condition. The following are some common ways to prevent refeeding syndrome or its risk factors:
- People at high risk of malnourishment should be assessed and treated beforehand. Intravenous nutrients, certain vitamins, and food or drink supplements should be administered under the supervision of a medical professional if proper intake of food orally is not possible.
- In case a person has undergone starving, fasting, or weight loss, the re-administration of proper diet should not be done abruptly. Slowly let your body adapt to eating normal food by starting with light low-carb meals.
- Regular blood test assessment and monitoring of electrolyte levels if alcohol or certain medications (e.g. antacids, chemotherapy drugs, diuretics) are used for the long-term, and if the person is at high risk of malnourishment from starvation, chronic disease, or weight loss.